Le Infezioni in Medicina, n. 4, 451-462, 2024
doi: 10.53854/liim-3204-4
REVIEW
Infectious disease outbreaks in the wake of natural flood disasters: global patterns and local implications
Jaime David Acosta-España1,2,3,4,5, Daniel Romero-Alvarez1,4, Camila Luna6, Alfonso J. Rodriguez-Morales6,7,8
1 Health Sciences Faculty, Universidad Internacional SEK (UISEK), Quito, 170120, Ecuador;
2 School of Medicine, Pontificia Universidad Católica del Ecuador, Quito, Ecuador;
3 Institute of Microbiology, Friedrich Schiller University Jena, Jena, Germany;
4 Research Group of Emerging and Neglected Diseases, Ecoepidemiology and Biodiversity, Health Sciences Faculty, School of Biomedical Sciences, Universidad Internacional SEK (UISEK), Quito 170120, Ecuador;
5 Centro de Investigación para la Salud en América Latina (CISeAL), Pontificia Universidad Católica del Ecuador, Quito, Ecuador;
6 Faculty of Health Sciences, Universidad Científica del Sur, Lima, 4861, Peru;
7 Grupo de Investigación Biomedicina, Faculty of Medicine, Fundación Universitaria Autónoma de las Américas-Institución Universitaria Visión de las Américas, Pereira, Risaralda 660003, Colombia;
8 Gilbert and Rose-Marie Chagoury School of Medicine, Lebanese American University, Beirut, P.O. Box 36, Lebanon
Article received 15 August 2024 and accepted 19 October 2024
Corresponding author
Jaime David Acosta-España
E-mail: jaime.acosta@uisek.edu.ec
SummaRY
Climate change is an urgent global health challenge, with floods becoming increasingly frequent and exacerbating the spread of infectious diseases. With its diverse climates and recurring natural disasters, Latin America is particularly susceptible to outbreaks following floods. These events disrupt ecosystems and create ideal conditions for the spread of waterborne and vector-borne pathogens. Floods also damage infrastructure, displace populations, and restrict access to clean water and healthcare services, further compounding public health risks. This review assesses the impact of floods on infectious disease outbreaks in Latin America, focusing on key epidemiological trends, vulnerabilities, and strategies for mitigation.
This narrative review aims to analyse the incidence and transmission of infectious diseases during and after floods in Latin America. Particular emphasis is placed on waterborne diseases, such as cholera and leptospirosis, vector-borne diseases, including dengue and malaria, and respiratory infections in displaced populations. The review also considers how socioeconomic factors, healthcare limitations, and climate vulnerabilities amplify the public health risks in flood-affected regions.
We extensively searched PubMed, Google Scholar, Scopus, Science Direct, and Web of Science from 2010 to May 2024, examining articles in English, Spanish, and Portuguese. The search focused on original descriptive studies on flooding and infectious diseases, particularly in Latin America. Keywords such as ‘flooding,’ ‘waterborne diseases,’ ‘vector-borne diseases,’ ‘skin and soft tissue infections,’ ‘respiratory infections,’ and specific disease names like leishmaniasis and malaria were employed. A descriptive analysis of the relevant articles was performed to synthesise the key findings.
The results show a clear association between floods and infectious disease outbreaks in several countries. Waterborne diseases, especially cholera and leptospirosis, are frequently reported following floods due to contaminated water. Vector-borne diseases like dengue and malaria see increased transmission as stagnant water forms ideal breeding grounds for mosquitoes. Respiratory infections are also prevalent in overcrowded, unsanitary shelters for displaced populations. Additionally, fungal infections and skin diseases are notable concerns, especially in areas with prolonged exposure to floodwaters.
Floods disproportionately affect vulnerable populations, particularly low-income areas with insufficient infrastructure and limited healthcare access. Climate change is likely to intensify the frequency and severity of floods further, increasing the health risks.
Finally, this review underscores the critical need for improved disaster preparedness, enhanced healthcare infrastructure, and better water and sanitation systems in flood-prone regions. Strengthening public health interventions and implementing climate adaptation strategies are essential to mitigating the impact of infectious diseases in future flood events.
Keywords: Infectious disease outbreaks, floods, vector-borne diseases, waterborne diseases, disaster preparedness.
INTRODUCTION
The global challenge of climate change has been reshaping health outcomes worldwide since then. Natural disasters are becoming increasingly frequent and severe [1]. According to the Intergovernmental Panel on Climate Change (IPCC), the frequency and intensity of extreme weather events have risen markedly over the past decade due to climate change [1]. Floods are now among the most common natural disasters globally, impacting millions of lives yearly [2].
The World Meteorological Organization (WMO) study reports that the last decade has seen some of the worst floods on record [3]. Notably, the 2014 Southeastern Europe floods, the 2018 Kerala floods in India, and the 2020 flooding in China’s Yangtze River basin have caused widespread devastation [3]. These events highlight the increasing vulnerability of various regions to severe flooding and underscore the urgent need for effective mitigation and response strategies.
Globally, floods have affected every continent, significantly impacting Asia, Africa, and the Americas [4-7]. In Asia, monsoon rains have caused catastrophic flooding in India, Bangladesh, and Pakistan. In Africa, seasonal floods have been recurrent in Nigeria and Mozambique [4-6]. The Americas have also seen substantial flooding, with the United States experiencing severe hurricanes and floods in states like Texas and Louisiana [8, 9].
Due to environmental, socioeconomic, and infrastructural factors, Latin America is highly susceptible to flooding. Countries like Brazil, Colombia, Peru, and Ecuador have frequently faced devastating floods. For instance, the 2017 Peru floods, caused by the El Niño Southern Oscillation (ENSO), affected over 1.1 million people and led to a surge in infectious diseases such as leptospirosis and dengue [10]. Similarly, Brazil’s floods in 2024 resulted in significant public health crises, with increases in waterborne and vector-borne diseases [11].
Flooding creates ideal conditions for the proliferation of infectious diseases. Contaminated water sources facilitate the spread of pathogens like Vibrio cholerae and Leptospira spp., leading to outbreaks of cholera and leptospirosis [12, 13]. Stagnant water provides breeding grounds for mosquitoes, increasing the risk of dengue, malaria, and Zika virus transmission [14]. Population displacement and overcrowded shelters also exacerbate the spread of respiratory infections and skin diseases [15].
Latin America is mainly affected by rapid urbanisation, inadequate sanitation, and insufficient healthcare infrastructure, factors that amplify the public health impact of flooding [15]. Climate variability, including El Niño and La Niña phenomena, further complicates efforts to predict and mitigate the effects of natural disasters [16].
This narrative review aims to synthesise current evidence on the relationship between floods and the risk of infectious diseases in Latin America. By analysing existing literature, the review highlights vital challenges, identifies knowledge gaps, and proposes recommendations for enhancing public health responses and resilience in climate-induced disasters like flooding.
METHODS
This narrative review aimed to synthesise current literature on the relationship between flooding and infectious diseases. We performed an extensive search across five major databases: PubMed, Google Scholar, Scopus, ScienceDirect, and Web of Science. The search spanned from 2010 to May 2024 and was conducted in three languages-English, Spanish, and Portuguese. We targeted original descriptive studies focused on infectious disease outbreaks associated with flooding. A wide range of search terms was used, including ‘flooding,’ ‘infectious diseases,’ ‘helminth,’ ‘vector-borne diseases,’ ‘waterborne diseases,’ ‘respiratory infections,’ ‘skin and soft tissue infections,’ and ‘fungal infections,’ in addition to specific disease names like ‘leishmaniasis’ and ‘malaria.’ The search strategy also incorporated broader keywords such as ‘natural disaster,’ ‘post-flooding,’ and ‘helminthic infection’.
Our initial search returned 2,367 articles. After removing duplicates, 1,134 unique articles remained for screening. Inclusion criteria for this review were:
1) studies that explored the relationship between flooding and infectious diseases;
2) articles involving human populations impacted by flood events;
3) research conducted in any region, with a focus on studies from the Americas;
4) original research articles, including observational and descriptive studies, that provided new data on infectious disease outbreaks related to flooding.
We applied exclusion criteria to refine our selection. Excluded articles were those that
1) addressed non-infectious outcomes;
2) were unrelated to flooding or its consequences;
3) were reviews, meta-analyses, or articles that did not contribute original data;
4) focused solely on the environmental or economic impacts of flooding without a connection to infectious diseases;
5) covered only modelling or policy aspects without discussing actual disease outbreaks.
These criteria ensured the inclusion of studies directly addressing the scope of this review.
After applying inclusion and exclusion criteria, 352 full-text articles were reviewed, and 44 studies were deemed appropriate for inclusion in the final analysis. These studies provided data on the impact of floods on various infectious diseases, including waterborne, vector-borne, respiratory, and skin infections. Special attention was given to studies from the Americas, where flood events and their public health implications are of particular concern.
We employed descriptive content analysis to analyse the findings of the selected studies. This method allowed us to categorise and interpret the studies, focusing on crucial aspects such as the types of pathogens involved, modes of disease transmission, and geographical variability in post-flood infectious disease outbreaks. By employing this approach, we aimed to capture the overall trends and patterns seen across multiple flood-related infectious disease events. The focus was on understanding the impact of floods on public health, particularly regarding disease spread, without conducting any diagnostic or statistical analysis.
This narrative review does not involve predictive modelling or statistical analysis. Instead, it offers a qualitative synthesis of the current knowledge, drawing connections between flooding events and infectious disease risks, especially in vulnerable regions like the Americas. Through this process, we aim to highlight the public health challenges flood-prone areas face and contribute to a better understanding of the relationship between natural disasters and infectious disease outbreaks.
RESULTS
Factors Influencing Disease Spread
Environmental Factors
Climate change is a significant environmental factor influencing the spread of infectious diseases, particularly in flood-prone regions. Alterations in climatic patterns lead to increased frequency and intensity of extreme weather events such as floods, which create breeding grounds for disease vectors like mosquitoes and contaminate water sources with pathogens. Poor sanitation and compromised water quality further exacerbate the transmission of waterborne diseases like cholera and leptospirosis [12, 17].
An analysis of 3,213 case examples identified 286 unique pathogenic diseases linked to climatic hazards, with 277 exacerbated by these events. Floods, particularly, aggravated 121 diseases, mainly through waterborne, vector-borne, and direct contact transmission. Flood-induced wastewater overflows often spread pathogens like norovirus, hantavirus, hepatitis, and Cryptosporidium. These events bring pathogens closer to people and push populations into unsafe conditions, increasing exposure risks. This combination significantly heightens infectious disease outbreaks following floods, with profound implications, especially in regions where infrastructure and healthcare systems are vulnerable [17].
Socioeconomic Factors
Socioeconomic conditions are crucial in determining vulnerability to disease outbreaks following floods. Poverty limits access to adequate housing, clean water, and healthcare services, increasing infection susceptibility [18]. Population displacement, a common consequence of flooding, disrupts social networks and healthcare access, further compounding the spread of diseases [15].
Healthcare System Response
The capacity, preparedness, and resilience of healthcare systems are critical in mitigating the impact of floods on public health. Effective disaster preparedness and response plans are essential to promptly address the surge in healthcare demand during and after flooding events. Building resilient healthcare infrastructures, ensuring adequate medical supplies, and enhancing healthcare access in flood-prone areas are crucial to improving disease management and reducing mortality rates [19]. Understanding and addressing these factors are essential for developing comprehensive strategies to mitigate floods’ public health impacts and improve resilience in vulnerable communities.
Impact of Climate Change on Infectious Disease Transmission and Migration
These environmental changes increase the likelihood of contact between humans and pathogens and enhance the survival and reproduction of these pathogens, particularly in higher latitudes where warmer winters allow vectors and pathogens to thrive year-round. Climatic hazards also exacerbate the risks by displacing human populations and forcing them closer to pathogens [20]. Heatwaves, storms, floods, and sea-level rise contribute to human migrations and displacements, often leading to crowded, unsanitary conditions where infectious diseases spread more easily [20].
Additionally, droughts force humans and animals to congregate around limited water sources, increasing the transmission of waterborne diseases like West Nile virus. These hazards bring people and pathogens closer and impair human immune responses through malnutrition, stress, and exposure to unsafe conditions, further compounding the risk of infectious disease outbreaks [20].
Vector-borne Diseases
The accumulation of water provides an ideal breeding ground for various vectors. Despite geographical variations in infectious disease epidemiology, systematic reviews such as Quintanilla’s have consistently shown the emergence of vector-borne diseases following floods globally [17, 21, 22]. Dengue fever is also a significant post-flood concern in Brazil, the Dominican Republic, and Haiti [21, 23].
Concerning geographic regions, other vector-borne diseases such as Rift Valley Fever, West Nile Virus, Japanese Encephalitis, Ross River virus, Barmah Forest virus, and Murray Valley encephalitis have also been reported following flooding events [24, 25]. Notably, studies indicate a post-event increase in malaria cases, underscoring the significant health risk of flooding [24].
For Latin America, it is paramount to analyse the potential occurrence of endemic diseases such as yellow fever, schistosomiasis, onchocerciasis, lymphatic filariasis, Zika, Chikungunya, leishmaniasis, Chagas disease [26]. These diseases can significantly impact populations in crowded shelters and areas with vector presence. Effective vector control measures and community-based preventive strategies are crucial to mitigating the transmission dynamics exacerbated by flooding events [22].
Waterborne Diseases
Studies from the United States have highlighted the detection of various waterborne infectious diseases following exposure to tropical cyclonic storms [27]. These include pathogen species such as Legionella, Cryptosporidium, Giardia, Shiga toxin-producing Escherichia coli, Salmonella, and Shigella. Tropical cyclonic storms, known for their intense rainfall and flooding, significantly increase the risk of pathogen-contaminated water sources, posing severe health threats to affected populations.
A Report from the Red Cross following floods in Pakistan has underscored the prevalence of diarrhoeal diseases among affected individuals [28]. The overcrowded living conditions in emergency shelters further exacerbate the spread of diseases like dysentery and cholera, which can rapidly escalate due to compromised hygiene and sanitation facilities.
Between 2012 and 2017, data from Malaysia highlighted bacterial food poisoning as the most reported waterborne disease, followed by leptospirosis, melioidosis, dysentery, and typhoid or paratyphoid fevers [29]. These findings show the diverse array of waterborne diseases prevalent in flood-affected regions.
Soil-transmitted helminth infections (STHs)
The most common parasites infecting humans globally are roundworms (Ascaris lumbricoides), whipworms (Trichuris trichiura), and hookworms (Ancylostoma duodenale and Necator americanus) [30, 31]. Collectively known as soil-transmitted helminths, they spread via ingesting eggs from infected individuals, contaminating soil and water sources, or through penetration of larvae hatched from the eggs [30, 31]. These STHs respond to similar anti-helminthic treatments and are diagnosed using the same laboratory methods (see Table 1) [30].
Table 1 - Aetiology, diagnoses, and first-line recommended treatments for frequent infectious and tropical floods-related diseases.
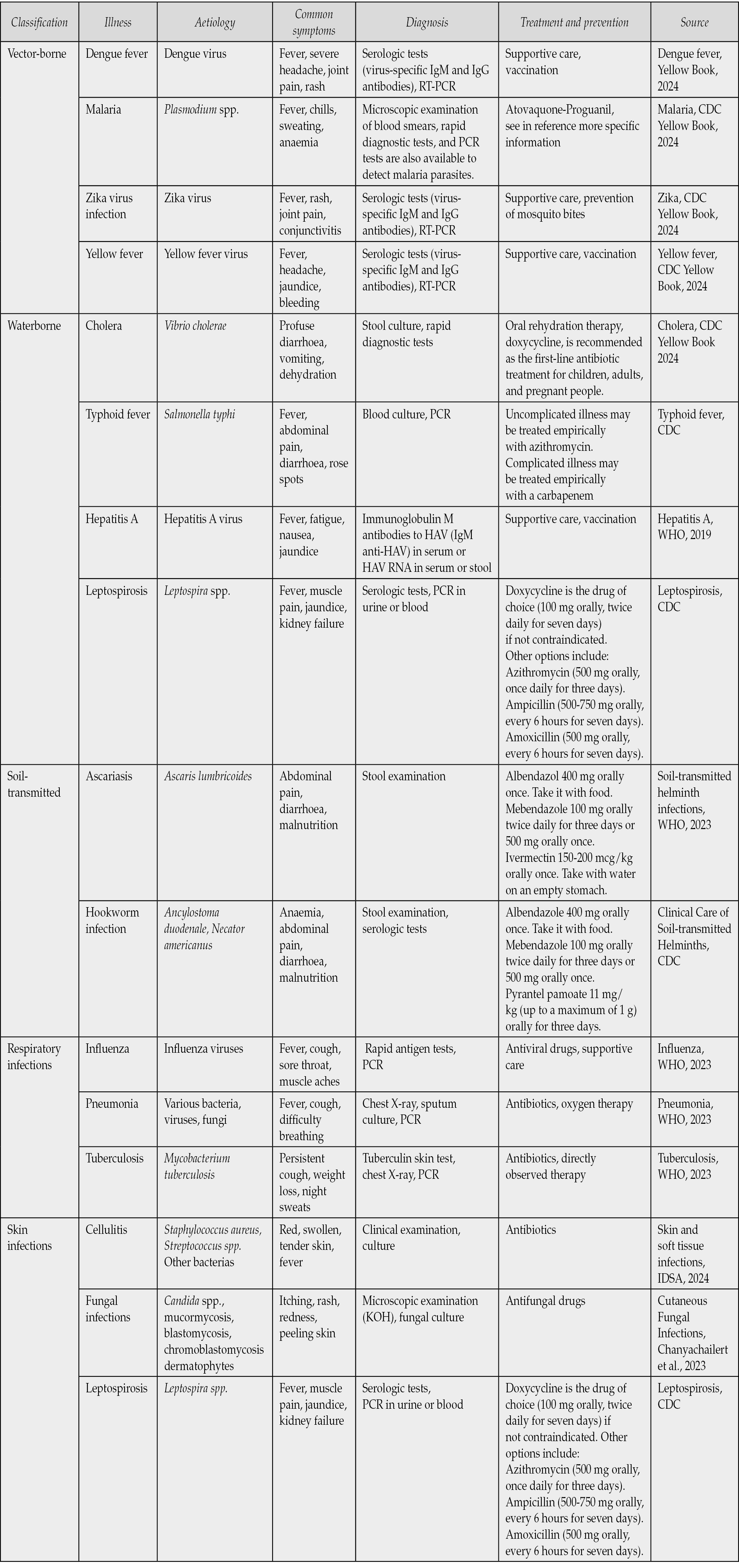
In a study conducted by Deka and colleagues in 2021 in India, it was found that among the paediatric population studied in a post-flood event, at least 16.3% presented with a helminth infection [32]. The detected parasites included Ascaris lumbricoides, hookworms, and Trichuris trichiura. Additionally, coinfections were identified in 3.9% of the study population, involving combinations such as Ascaris plus hookworm, Ascaris plus Trichuris, and Hookworm plus Trichuris. Remarkably, 0.9% of cases exhibited triple infection by Ascaris, hookworm, and Trichuris [32].
In flood-prone Myanmar, a prevalence of at least 24% for helminth infections was found. A. lumbricoides, T. trichiura, and S. stercoralis accounted for 14% of cases, with a higher incidence observed in cities near rivers. Non-geohelminths such as taeniasis, Schistosoma spp. and Paragonimus spp. were also detected [33].
After the 2016 floods in Sri Lanka, a faecal study in children did not detect STHs in the analysed samples [34]. Possible reasons for this finding include low parasite loads, limitations of diagnostic techniques, specific geographical areas studied, or a decline in these infections in Sri Lanka [35]. Post-flooding comprehensive hygiene and sanitation interventions might avert parasitic disease transmission to basal burdens [36].
Respiratory Infections
Respiratory infections driven by overcrowding in temporary shelters and compromised hygiene conditions might trigger outbreaks of influenza, pneumonia, and tuberculosis, which escalate in incidence under such circumstances (see Table 1) [37]. In one of the worst floods in Bangladesh in 1988, respiratory infections ranked second after diarrhoea, affecting 17.4% of the affected population and resulting in a mortality rate of 13% [38]. In a systematic review focused on the 2019 floods in Iran, there were alerts regarding the possibility of an increase in influenza, respiratory syncytial virus, and adenovirus [39]. Meanwhile, Allied and colleagues, in their analysis of floods in Pakistan in 2022, also warned about the potential impact of Coronavirus Disease 2019 (COVID-19) [40].
Following heavy flooding, individuals face an increased risk of preventable bacterial respiratory infections. The crowded conditions in temporary shelters, lack of access to healthcare services, and poor hygiene can facilitate the spread of diseases such as diphtheria, pertussis (whooping cough), and pneumonia caused by Haemophilus influenzae type b (Hib) and Streptococcus pneumoniae. Diphtheria and pertussis are highly contagious and can have serious consequences, especially for young children and unvaccinated individuals. Pneumococcal pneumonia and Hib infection can lead to severe complications, including meningitis and bacteremia, which are challenging to manage in resource-limited environments. Timely and appropriate vaccination is crucial to prevent outbreaks of these diseases in disaster-affected populations [41].
On the other hand, despite not being an acute infection, patients with active tuberculosis without a prior diagnosis may present symptoms due to worsening nutritional conditions. It is essential to bear in mind that these patients with pre-existing chronic cough could have tuberculosis and would pose a risk to other refugees. Furthermore, countries with endemic tuberculosis should plan to monitor populations that shared shelters and were in overcrowded conditions [42].
Skin and Soft Tissue Infections
In flood situations, the risk of skin infections increases significantly due to exposure to contaminated water and trauma from debris. During such events, injuries from sharp objects hidden in murky floodwaters or from clinging to structures during rescue attempts can lead to open wounds prone to infection [43]. An article by Bandino and colleagues discusses the likelihood of infection from agents such as Staphylococcus and Streptococcus. Additionally, bacteria associated with specific risks, such as those found in marine environments (e.g., Vibrio vulnificus) or freshwater (e.g., Aeromonas hydrophila), may also be present. In cases of contamination with sewage water, even bacteria like Burkholderia could be encountered, potentially exhibiting antibiotic resistance factors [44].
In flood-affected areas, the risk of leptospirosis significantly increases due to exposure to contaminated water sources harbouring Leptospira interrogans, particularly after heavy rains or flooding events that overwhelm sewage systems [45]. Leptospirosis, a zoonotic disease primarily transmitted through contact with the urine of infected animals like rodents, thrives in warm freshwater environments, with tropical regions showing the highest incidence. Following floods, outbreaks of leptospirosis have been extensively documented globally, including notable instances in Hawaii and other areas where floods caused by typhoons led to thousands of cases [46].
Fungal Infections
Numerous fungal infections are prevalent in flood and disaster settings. Chromoblastomycosis, caused by dematiaceous fungi such as Fonsecaea pedrosoi, typically emerges in tropical regions following traumatic inoculation from decaying plant material. Its diagnosis poses challenges due to its resemblance to other disease conditions [47]. Blastomycosis, caused by Blastomyces dermatitidis, primarily manifests as a pulmonary disease but can also present with cutaneous lesions resembling squamous cell carcinoma, particularly in moist environments post-flooding [48, 49]. Mucormycosis, caused by Mucorales fungi, leads to severe, necrotising infections primarily in immunocompromised individuals, often following traumatic injuries during disaster scenarios [50-52]. Lastly, dermatophytosis, common in flooded areas due to increased environmental exposure, presents as a superficial fungal infections [53]. Prompt diagnosis and appropriate antifungal therapy play a crucial role in managing these infections amidst disaster-related challenges
DISCUSSION
The evidence synthesised from various studies demonstrates that flooding significantly amplifies the transmission of infectious diseases through multiple pathways. These include the creation of favourable environments for disease vectors and the contamination of water supplies. As a result, the prevalence of diseases such as malaria, dengue fever, cholera, and leptospirosis is markedly elevated in regions affected by flooding [4, 12, 33, 43].
In Latin America, the impact on public health is pronounced due to socioeconomic disparities, inadequate infrastructure, and geographical vulnerability. Recurrent outbreaks of diseases like dengue and Zika, which thrive in stagnant water, coupled with poor sanitation infrastructure, disproportionately affect marginalised communities lacking access to clean water and healthcare services [2, 7, 39, 54]. There is an urgent need for targeted public health interventions considering local epidemiological patterns and socioeconomic realities to curb disease transmission in flood-prone areas.
Moreover, Latin America shares commonalities with other flood-prone regions regarding post-flooding disease patterns. However, endemic diseases, such as yellow fever and Chagas disease prevalence, suggest the development of specific public health responses. Effectively addressing these issues demands strengthening healthcare systems, enhancing sanitation, and developing robust disaster preparedness plans that align with local conditions to bolster resilience against health threats associated with flooding [12, 28, 33].
Significant challenges persist, including insufficient healthcare resources, limited access to safe drinking water and sanitation, and inadequacies in disaster preparedness frameworks. These shortcomings highlight the critical need for improved epidemiological surveillance, thorough data collection on disease burden, and a better understanding of transmission dynamics specific to post-flooding contexts in Latin America. Future research should prioritize evaluating the effectiveness of various intervention strategies, assessing the socioeconomic consequences of flooding, and fostering resilience in vulnerable communities to prepare for potential future flood events.
The recent flooding events in Latin America, exemplified by the 2023 floods in Brazil and the 2024 floods in Ecuador, have highlighted the urgent need for robust public health responses to mitigate the rising threat of infectious diseases [55]. This situation is exacerbated by the interplay of climate change, which is projected to increase the frequency and intensity of extreme weather events, placing additional pressure on vulnerable populations [12].
Addressing the intersecting issues of flooding and infectious diseases demands a holistic approach encompassing disaster preparedness, surveillance, healthcare provision, and community engagement. Urgent action is imperative to mitigate the health consequences of flooding and safeguard the well-being of vulnerable populations (Figure 1 shows flood-affected regions until July 2024).
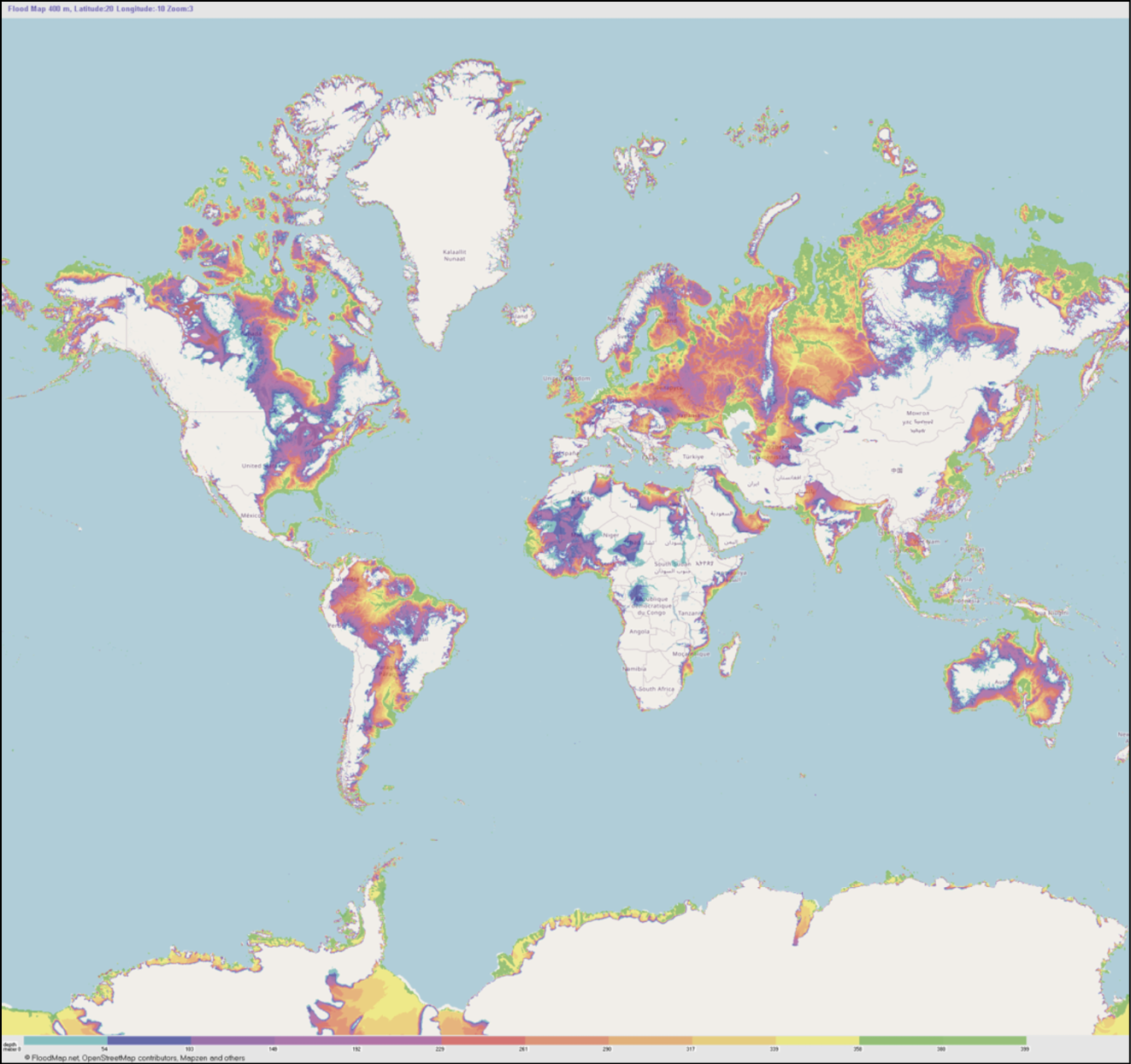
Figure 1 - Worldwide flood heatmap, 2024.
This figure shows global flooding up to July 2024.
Data Sources: Mazpzen, TNM, SRTM, GMTED, ETOPO1, FloodMap.
Moreover, enhancing sanitation and access to clean water must be prioritised [5, 32, 37]. Sustainable water management practices and infrastructure development can mitigate the risk of waterborne diseases in flood-prone areas [28]. Implementing effective vector control measures is also vital, particularly in regions prone to dengue and Zika outbreaks [11, 24, 26, 38, 56]. Community-based approaches, such as involving local residents in vector surveillance and control activities, can foster greater resilience and ensure that interventions are culturally relevant and practical [12].
Establishing comprehensive disaster preparedness plans tailored to the unique epidemiological profiles of local communities is essential. These plans should include clear protocols for disease surveillance, rapid response strategies to manage outbreaks, and data collection and sharing mechanisms to inform public health decisions. Enhancing collaboration among governmental, non-governmental, and international organisations can facilitate resource sharing and promote a coordinated response to flooding-related health threats [43, 57].
Flooding significantly heightens the risk of infectious diseases in Latin America due to three main factors. Firstly, floods often contaminate water sources with sewage, leading to the spread of waterborne diseases like cholera, leptospirosis, and hepatitis A. Poor sanitation infrastructure in many affected areas exacerbates this risk. Secondly, standing water from floods creates ideal breeding grounds for mosquitoes, increasing the incidence of vector-borne diseases such as dengue, Zika, and malaria. The warm climate in much of Latin America further supports mosquito proliferation after floods. Thirdly, disruptions to healthcare systems and displacement of populations during flood events can hinder access to medical care and vaccination, reducing the capacity to control outbreaks. Vulnerable populations, including those living in informal settlements, are especially at risk due to overcrowded conditions and limited resources, making it difficult to mitigate the spread of infections. The combination of water contamination, increased mosquito breeding, and healthcare disruptions creates a complex public health challenge, making flood-prone areas in Latin America particularly susceptible to infectious disease outbreaks.
Furthermore, future research must focus on understanding the complex interplay between environmental factors, socioeconomic determinants, and disease transmission dynamics in post-flooding scenarios. This knowledge will be invaluable in developing targeted interventions adaptable to the evolving landscape of climate change and its impact on health.
CONCLUSIONS
The recent flooding events in Latin America and other flood-prone regions highlight the complex intersection of climate change, environmental health risks, and public health resilience. There is an urgent need for coordinated efforts to strengthen disaster preparedness, enhance healthcare infrastructure, and implement targeted interventions that address local infectious disease dynamics. By prioritising proactive measures, such as early warning systems, vector control strategies, and community engagement, stakeholders can mitigate the health impacts of floods and safeguard vulnerable populations. Continued research into the socioeconomic effects of flooding on disease vulnerability and the effectiveness of intervention strategies is crucial for informing evidence-based policies and building resilient health systems. Ultimately, a holistic approach is essential to mitigate the growing health threats of climate-induced floods and ensure sustainable public health outcomes in the face of escalating environmental challenges.
Limitations
This review’s limitations stem from the complexities inherent in studying the intersection of floods and infectious diseases, particularly in the context of Latin America. While we employed a comprehensive search strategy across multiple English, Spanish, and Portuguese databases from 2010 to May 2024, the reliance on available literature may have introduced selection bias. Not all relevant studies may have been captured, particularly those published in non-indexed journals or languages not included in our search.
Additionally, the heterogeneity of study designs and methodologies limits the comparability of findings across different regions and disease contexts. Variations in data collection techniques, case definitions, and diagnostic methods can affect the reported incidence and prevalence of flooding-related diseases. Furthermore, the emphasis on descriptive articles may have restricted our ability to draw definitive causal inferences regarding the impact of floods on infectious disease transmission.
The socioeconomic factors influencing disease vulnerability are multifaceted and can vary significantly within and between communities. While we addressed these factors, the complexity of interactions among socioeconomic status, healthcare access, and public health infrastructure may not have been fully captured in the existing literature. Furthermore, the impact of climate change on flood patterns and subsequent disease outbreaks is an evolving area of research, and the studies included in this review may not reflect the latest trends or emerging infectious diseases linked to floods.
Lastly, while we aimed to synthesise findings relevant to Latin America, the generalisability of our conclusions may be limited. Each country’s unique socioeconomic, cultural, and environmental contexts necessitate tailored public health interventions. Future research should focus on longitudinal studies that assess the long-term health impacts of flooding events and the effectiveness of intervention strategies in diverse settings. A deeper understanding of these limitations will be crucial in informing evidence-based policies and improving preparedness for future flood-related health challenges.
Conflicts of interest
None to declare
Funding
No specific funding was received for this publication. We thank the universities of the authors of this manuscript for supporting the research.
Acknowledgements
We sincerely thank those who contributed to this manuscript, especially the Universidad Particular Internacional SEK del Ecuador, Pontificia Universidad Católica del Ecuador, and Friedrich-Schiller-Universität Jena. JDA-E idealised the main idea, wrote the initial manuscript, conducted the narrative review and synthesised the data. DR-A reviewed all versions, contributed to the writing of the initial manuscript and provided in-depth analysis to improve the manuscript. CL contributed revisions and edits to all versions of the manuscript. AJR-M supervised, edited and contributed to the initial concept idea of the manuscript.
REFERENCES
[1] Intergovernmental Panel on Climate Change. Climate Change 2021: The Physical Science Basis | Climate Change 2021: The Physical Science Basis, https://www.ipcc.ch/report/ar6/wg1/ (2021, accessed 10 July 2024).
[2] Aerts JCJH, Botzen WJ, Clarke KC, et al. Integrating human behaviour dynamics into flood disaster risk assessment. Nat Clim Change. 2018; 8: 193-199.
[3] World Meteorological Organization. Statement to SBSTA 52-55, https://library.wmo.int/doc_num.php?explnum_id=10833 (2021).
[4] Umar N, Gray A. Flooding in Nigeria: a review of its occurrence and impacts and approaches to modelling flood data. Int J Environ Studies. 2023; 80: 540-561.
[5] Mirza MMQ. Climate change, flooding in South Asia and implications. Reg Environ Change. 2011; 11: 95-107.
[6] Swain S, Taloor AK, Dhal L, et al. Impact of climate change on groundwater hydrology: a comprehensive review and current status of the Indian hydrogeology. Applied Water Science. 2022; 12:6 2022; 12: 1-25.
[7] Espinoza JC, Ronchail J, Frappart F, et al. The Major Floods in the Amazonas River and Tributaries (Western Amazon Basin) during the 1970-2012 Period: A Focus on the 2012 Flood. J Hydrometeorol. 2013; 14: 1000-1008.
[8] Smith AB, Katz RW. US billion-dollar weather and climate disasters: Data sources, trends, accuracy and biases. Natural Hazards. 2013; 67: 387-410.
[9] Emanuel K. Assessing the present and future probability of Hurricane Harvey’s rainfall. Proc Natl Acad Sci U S A. 2017; 114: 12681-12684.
[10] Yglesias-González M, Valdés-Velásquez A, Hartinger SM, et al. Reflections on the impact and response to the Peruvian 2017 Coastal El Niño event: Looking to the past to prepare for the future. PLoS One; 18. Epub ahead of print 1 September 2023. DOI: 10.1371/JOURNAL.PONE.0290767.
[11] Martins-Filho PR, Croda J, de Souza Araújo AA, et al. Catastrophic Floods in Rio Grande do Sul, Brazil: The Need for Public Health Responses to Potential Infectious Disease Outbreaks. Rev Soc Bras Med Trop. 2024; 57: e00603-2024.
[12] Few R, Ahern M, Matthies F, et al. Floods, health and climate change: a strategic review. Epidemiol Rev. 2005; 27: 36-46.
[13] Cann KF, Thomas DR, Salmon RL, et al. Extreme water-related weather events and waterborne disease. Epidemiol Infect. 2013; 141: 671-686.
[14] World Health Organization. Vector-borne diseases, https://www.who.int/news-room/fact-sheets/detail/vector-borne-diseases (2020, accessed 10 July 2024).
[15] Connolly MA, Gayer M, Ryan MJ, et al. Communicable diseases in complex emergencies: Impact and challenges. Lancet. 2004; 364: 1974-1983.
[16] Anyamba A, Chretien JP, Britch SC, et al. Global Disease Outbreaks Associated with the 2015-2016 El Niño Event. Scientific Reports. 2019 9:1 2019; 9: 1-14.
[17] Mora C, McKenzie T, Gaw IM, et al. Over half of known human pathogenic diseases can be aggravated by climate change. Nature Climate Change. 2022 12:9 2022; 12: 869-875.
[18] Montgomery MR. The urban transformation of the developing world. Science (1979). 2008; 319: 761-764.
[19] Patt A, Glantz MH. Currents of Change: Impacts of El Nino and La Nina on Climate and Society. Int J Afr Hist Stud. 2001; 34: 173.
[20] Mora C, McKenzie T, Gaw IM, et al. Over half of known human pathogenic diseases can be aggravated by climate change. Nature Climate Change. 2022 12:9 2022; 12: 869-875.
[21] Quintanilla N. Outbreaks of Vector-borne Infectious Disease Following a Natural Disaster. Georgetown Medical Review; 6. Epub ahead of print 21 December 2022. DOI: 10.52504/001C.38768.
[22] Confalonieri UE, Suassuna Dutra FR. Climate Change and Vector Borne Diseases in Latin America. Environmental Deterioration and Human Health: Natural and Anthropogenic Determinants 2014; 9789400778900: 315-324.
[23] Ricardo-Rivera SM, Aldana-Carrasco LM, Lozada-Martinez ID, et al. Mapping Dengue in children in a Colombian Caribbean Region: clinical and epidemiological analysis of more than 3500 cases. Infez Med. 2022; 30: 602-609.
[24] Coalson JE, Anderson EJ, Santos EM, et al. The Complex Epidemiological Relationship between Flooding Events and Human Outbreaks of Mosquito-Borne Diseases: A Scoping Review. Environ Health Perspect; 129. Epub ahead of print 1 September 2021. DOI: 10.1289/EHP8887.
[25] D’amore C, Grimaldi P, Ascione T, et al. West Nile Virus diffusion in temperate regions and climate change. A systematic review. Infez Med. 2023; 31: 20-30.
[26] Joob B, Wiwnaitkit V. Mapping Zika by Geographic Information System. Infez Med. 2018; 26: 295.
[27] Lynch VD, Shaman J. Waterborne Infectious Diseases Associated with Exposure to Tropical Cyclonic Storms, United States, 1996-2018. Emerg Infect Dis. 2023; 29: 1548.
[28] British Red Cross. Risk of waterborne disease after Pakistan floods, https://www.redcross.org.uk/stories/disasters-and-emergencies/world/risk-of-waterborne-disease-after-pakistan-floods (2023, accessed 10 July 2024).
[29] Shafii NZ, Saudi ASM, Pang JC, et al. Association of Flood Risk Patterns with Waterborne Bacterial Diseases in Malaysia. Water. 2023; 15: 2121.
[30] Jourdan PM, Lamberton PHL, Fenwick A, et al. Soil-transmitted helminth infections. Lancet. 2018; 391: 252-265.
[31] De Silva NR, Brooker S, Hotez PJ, et al. Soil-transmitted helminth infections: Updating the global picture. Trends Parasitol. 2003; 19: 547-551.
[32] Deka S, Barua D, Bahurupi Y, et al. Assessment of the Prevalence of Soil-Transmitted Helminth Infections and Associated Risk Factors among School-Aged Children in a Flood-Affected Area of Northeast India. Am J Trop Med Hyg. 2021; 105: 480.
[33] Han KT, Wai KT, Aye KH, et al. Emerging neglected helminthiasis and determinants of multiple helminth infections in flood-prone township in Myanmar. Trop Med Health. 47. Epub ahead of print 4 January 2019. DOI: 10.1186/S41182-018-0133-6.
[34] Ubhayawardana N, Gammana Liyanage I, Herath HMJCB, et al. Direct Microscopy of Stool Samples for Determining the Prevalence of Soil-Transmitted Helminthic Infections among Primary School Children in Kaduwela MOH Area of Sri Lanka following Floods in 2016. J Environ Public Health; 2018. Epub ahead of print 2018. DOI: 10.1155/2018/4929805.
[35] Gunawardena S, Gunawardena NK, Kahathuduwa G, et al. Integrated School-Based Surveillance for Soil-Transmitted Helminth Infections and Lymphatic Filariasis in Gampaha District, Sri Lanka. Am J Trop Med Hyg. 2014; 90: 661.
[36] Legge H, Pullan RL, Sartorius B. Improved household flooring is associated with lower odds of enteric and parasitic infections in low- and middle-income countries: A systematic review and meta-analysis. PLOS Global Public Health; 3. Epub ahead of print 1 December 2023. DOI: 10.1371/JOURNAL.PGPH.0002631.
[37] The Lancet Respiratory Medicine. Flooding and excessive rainfall risk respiratory health. Lancet Respir Med. 2024; 12: 89.
[38] Siddique AK, Baqui AH, Eusof A, et al. 1988 floods in Bangladesh: pattern of illness and causes of death. J Diarrhoeal Dis Res. 1991; 9: 310-314.
[39] Yavarian J, Shafiei-Jandaghi NZ, Mokhtari-Azad T. Possible viral infections in flood disasters: a review considering 2019 spring floods in Iran. Iran J Microbiol. 2019; 11: 85.
[40] Alied M, Salam A, Sediqi SM, et al. Disaster after disaster: the outbreak of infectious diseases in Pakistan in the wake of 2022 floods. Ann Med Surg. 2024; 86: 891.
[41] Jafari N, Shahsanai A, Memarzadeh M, et al. Prevention of communicable diseases after disaster: A review. J Res Med Sci. 2011; 16: 956.
[42] Basaria AAA, Ahsan A, Nadeem A, et al. Infectious diseases following hydrometeorological disasters: current scenario, prevention, and control measures. Ann Med Surg. 2023; 85: 3778.
[43] Tempark T, Lueangarun S, Chatproedprai S, et al. Flood-related skin diseases: a literature review. Int J Dermatol. 2013; 52: 1168-1176.
[44] Bandino JP, Hang A, Norton SA. The Infectious and Noninfectious Dermatological Consequences of Flooding: A Field Manual for the Responding Provider. Am J Clin Derm. 2015; 16: 399-424.
[45] Bierque E, Thibeaux R, Girault D, et al. A systematic review of Leptospira in water and soil environments. PLoS One; 15. Epub ahead of print 1 January 2020. DOI: 10.1371/JOURNAL.PONE.0227055.
[46] Leptospirosis After Flooding of a University Campus -- Hawaii, 2004: EBSCOhost, https://web.p.ebscohost.com/ehost/detail/detail?vid=0&sid=a5f27d5a-7372-4cb2-ab29-c64dc78aa06f%40redis&bdata=Jmxhbmc9ZXMmc2l0ZT1laG9zdC1saXZl#AN=20001665&db=aph (accessed 11 July 2024).
[47] Wiebels D. Chromomycosis: late sequela of the tsunami of 2004. Dermatol Pract Concept. 14.
[48] Klein BS, Vergeront JM, Disalvo AF, et al. Two outbreaks of blastomycosis along rivers in Wisconsin. Isolation of Blastomyces dermatitidis from riverbank soil and evidence of its transmission along waterways. Am Rev Respir Dis. 1987; 136: 1333-1338.
[49] Saccente M, Woods GL. Clinical and Laboratory Update on Blastomycosis. Clin Microbiol Rev. 2010; 23: 367.
[50] Snell BJ, Tavakoli K. Necrotizing fasciitis caused by Apophysomyces elegans complicating soft-tissue and pelvic injuries in a tsunami survivor from Thailand. Plast Reconstr Surg. 2007; 119: 448-449.
[51] Andresen D, Donaldson A, Choo L, et al. Multifocal cutaneous mucormycosis complicating polymicrobial wound infections in a tsunami survivor from Sri Lanka. Lancet. 2005; 365: 876-878.
[52] Acosta-España JD, Voigt K. Mini Review: Risk assessment, clinical manifestation, prediction, and prognosis of mucormycosis: implications for pathogen- and human-derived biomarkers. Front Microbiol. 2022; 13: 1-12.
[53] SH L, CP C, HC E, et al. Skin problems after a tsunami. J Eur Acad Dermatol Venereol. 2006; 20: 860-863.
[54] Kondo H, Seo N, Yasuda T, et al. Post-flood--infectious diseases in Mozambique. Prehosp Disaster Med. 2002; 17: 126-133.
[55] The Guardian. Disease and hunger soar in Latin America after floods and drought, study finds, https://www.theguardian.com/environment/article/2024/may/08/disease-hunger-soar-latin-america-floods-drought-study (2024, accessed 14 May 2024).
[56] Morin CW, Comrie AC, Ernst K. Climate and dengue transmission: Evidence and implications. Environ Health Perspect, 2013; 121: 1264-1272.
[57] Calonge N, Brown L, Downey A. Evidence-Based Practice for Public Health Emergency Preparedness and Response. JAMA. 2020; 324: 629.