Le Infezioni in Medicina, n. 4, 544-553, 2024
doi: 10.53854/liim-3204-14
INFECTIONS IN THE HISTORY OF INFECTIOUS DISEASES
A brief history of Guinea worm research in the modern period, 1698-1931
Jonathan David Roberts
School of Biology, University of Leeds, LS2 9JT, England
Article received 29 September 2023 and accepted 26 October 2024
Corresponding author
Jonathan David Roberts
E-mail: j.d.roberts@leeds.ac.uk
SummaRY
Guinea worm is a debilitating waterborne parasitic disease with a long history. This paper examines the ways guinea worm was understood in English-language scientific literature between 1688 and 1931. In the early eighteenth century, guinea worm was principally understood by English-speaking physicians as an exotic wonder of faraway lands. It became viewed as an African disease over the course of the eighteenth century, as transatlantic slavery exposed enslaved Africans to infection with the worm. Worms acquired in West Africa often emerged after arrival to the Caribbean, where the disease briefly established local transmission. However, British medicine only began to take any significant interest in guinea worm in the early nineteenth century, as British and British-employed troops in India began to contract the worm. This resulted in knowledge and specimens of guinea worm travelling to Britain, where they were used to develop the new science of zoology through the nineteenth century. Zoologists elsewhere, particularly in Germany, benefitted from British-Indian knowledge, which allowed Russian parasitologist Alexei Fedchenko to discover the full mechanism of guinea worm’s transmission in Samarkand. This zoological knowledge, and zoological view of guinea worm, was then incorporated into the emerging tropical medicine of the 1890s and twentieth century. A long history of guinea worm therefore provides important insights into the circulation of knowledge along imperial networks, and into the history of tropical medicine and parasitology.
Keywords: Guinea worm; dracunculiasis; dracontiasis; neglected tropical diseases; history of medicine; history of science; helminthiases; waterborne diseases.
INTRODUCTION
Guinea worm disease (dracunculiasis) is the subject of many legends, but few histories. Take, for instance, the story that the origin of the medical caduceus, a snake wrapped around a staff, is guinea worm, a worm wrapped around a stick (which remains the only method of extracting it from the body); or that guinea worm was the Biblical ‘fiery serpent’ which tormented the Hebrews in the desert (Numbers 21: 5-9) [1, 2]. The latter claim, originating with the biblical commentator Thomas Bartholin, was elaborated by the nineteenth-century German parasitologist Frederick Küchenmeister [3]. Neither claim is easy to verify or disprove, but they illustrate that the little dragon of Medina (Dracunculus medinensis) is as much a creature of medical mythology as a disease.
Despite recent interest, the history of guinea worm remains poorly described [2, 4-6]. In this journal, Simonetti et al have recently provided an excellent overview of dracunculiasis in ancient, medieval and early modern Europe and the Mediterranean, but only a brief sketch of the disease’s history after 1700, and they neglect its history in Africa (outside of Egypt), the Caribbean, India and Central Asia entirely [7]. This period from 1700 to 1931, I contend, was a crucial one for evolving scientific understandings of guinea worm in Europe, being a period in which guinea worm captured the medical imagination of Europe. Likewise, it is necessary to consider European encounters with guinea worm arising from transatlantic slavery, through which it gained the name it carries to this day, and its later entanglement with British-Indian medicine. This paper, based on a survey of the available English-language literature on guinea worm between 1698 and 1931, offers a brief overview of medical knowledge about this parasite in the English-speaking scientific world.
I trace the history of guinea worm in its key period as an object of medical research through published English-language scientific works on the disease complemented by items from the London School of Hygiene and Tropical Medicine archive and texts in other European languages.
Dracunculus medinensis is a nematode parasite of humans and other mammals. The first-stage larvae inhabit stagnant water, where they are ingested by the copepod crustaceans I will for the sake of clarity refer to as cyclops. Cyclops was once considered a single genus, but this is no longer the case, and Metacyclops, Thermocyclops and Mesocyclops in particular are known to be intermediate hosts of guinea worm [8]. Guinea worm larvae grow within the cyclops through two further larval stages before humans or animals drink water containing the cyclops. Following this, the larval worms emerge from the now-dissolved cyclops and enter the body cavity where they mature and mate. The males rapidly die off, but after a year, the female moves towards the surface of the body, emerging through a blister. When the victim enters water, the female releases larvae back into the water. This blister and the emergence of the worm causes temporary (or more rarely, permanent) disability, but dracunculiasis is very rarely fatal – though secondary infections of the blister may be.
GUINEA WORM AS A CURIOSITY
As Simonetti et al emphasise, guinea worm has often been defined as a curiosity rather than a problem [7]. At the opening of the eighteenth century guinea worm was seen as a strange phenomenon of exotic lands. London ‘chymist’ R. Clark, for instance, described dracunculiasis in 1698 as produced by drinking from a river ‘near Boghar a Citie of the Zagathaian Tartars’ [9]. Placed amid tales of witchcraft and hearts leaping from the chests of corpses, this epitomises the exotic and wondrous nature of guinea worm, something underlined by its appearance in the distant lands of the Tartars. Bukhara has a special place in the history of dracunculiasis, being the first place where the disease was eradicated (see below), but to Clark it was merely a strange land of the East, where you might expect such wonders as a worm-generating river [10, 11]. More educated authors, meanwhile, encountered guinea worm in the pages of ancient and medieval texts as the Dracunculus or Vena Medinensis. Learned writers such as John Freind, William Hillary and J. Browne referenced a range of Greek, Roman and Arabic authors such as Galen, Aetius, Avicenna, Rhazes and Albucasis when discussing guinea worm [12-14]. The connecting of Galen’s Dracunculus to the Irk medini of Arabic literature may originate with Engelbertus Kaempfer, whose encounters with guinea worm in Ormus (Bandar Abbas) and Tartary (central Asia) were frequently referenced by eighteenth-century authors [12, 13, 14-18]. Guinea worm was defined by its ancient heritage and its location in the distant lands of Arabia, Persia and Tartary, and several authors further referred to it occurring in the similarly exoticised lands of Ethiopia and India [12, 17, 19-21]. Throughout the eighteenth century, the tone of writings about guinea worm was one of curiosity. It was seen as ‘strange’, ‘remarkable’ or ‘extraordinary’, with stranger details, like the worm having two heads, occasionally added [19, 21, 22]. Daniel Turner’s 1732 Art of Surgery, furthermore, included ‘a much stranger Account’ of the disease ‘at Fort St. George in the East-Indies’ [19]. It was seen as an exotic wonder, rather than a serious problem for British medicine.
TRANSATLANTIC SLAVERY AND GUINEA WORM IN WEST AFRICA
Readers of ancient texts knew guinea worm occurred in the distant lands of Ethiopia; but eighteenth-century observers increasingly encountered it in West Africa and the West Indies, as enslaved Africans forced to drink contaminated water in slave forts manifested the worm only after they reached the Caribbean [14, 23]. Guinea worm spread as part of transatlantic slavery, which formed an ecological bridge across the Atlantic in the form of a massive, constant, but largely unidirectional, flow of human beings – creating the peculiar phenomenon of a disease endemic to the West Indies, but rarely acquired there. As the century progressed, poor water provision on Caribbean plantations allowed pools and wells in several areas such as Barbados and Grenada to become infected, fully transplanting yet another Old World disease into the New. As McNeill has demonstrated through his analysis of yellow fever, the reshaping of the ecologies of the West Indies and the Atlantic World brought by transatlantic slavery allowed diseases to thrive where they had never previously existed [24]. Guinea worm became associated with slavery – and acquired the name it carries to this day – because transatlantic slavery produced ideal conditions for its transmission.
This connection between guinea worm and West Africa, which would eventually result in it being defined as an African disease, was established early on. In 1707 naturalist and physician Hans Sloane identified Kaempfer’s Dracunculus persarum with the worms tormenting enslaved workers in the West Indies, while Kaempfer himself described Dracunculus as brought and produced from the Gold Coast (Ghana) (‘Guineenses nigritae lingua sua Meinensi vermes Ickon, ut produnt reduce ex auifero, illo Africae littore’) [15, 17]. Nicholas Andry, though referring to the guinea worm as ‘Silk Worms’, remarked in 1701 that ‘the African Negroes are subject to them’, and relays accounts of an enslaved ‘Ethiopian’ child manifesting the worm in Thessalonica and a Dutch soldier manifesting twenty-three worms in the West Indies [21]. In 1726 Richard Towne recorded that guinea worm
‘takes its Name from that Division of Africa which is called Guinea, because the Natives of that Country are very much subject to be infested with this Sort of Worm.’ [18]
It has been claimed that the name ‘guinea worm’ was coined by the mid-19th century colonial administrator John Tennent but the name was widely used a hundred years earlier [5, 7]. Indeed, there was a broad consensus amongst physicians by the middle of the eighteenth century that dracunculiasis was not a New World disease, but an African disease that only occurred in the West Indies via importation inside enslaved Africans. It became commonplace to define guinea worm as, in Erasmus Darwin’s phrase, ‘a thin worm brought from the coast of Guinea’ [25]. Dracunculiasis even appears in abolitionist (anti-slavery) literature as an evil endured by Africans and propagated by slavery [26, 27]. No less a figure than the architect of ‘the first randomised controlled trial’, James Lind, commented that it ‘seems in a manner most peculiar to Africa’, and medical writers who were not conversant with Avicenna increasingly defined the worm as a disease of Africans – and therefore of little importance [28, 29].
SLAVERY AND GUINEA WORM IN THE CARIBBEAN
It was in this context that guinea worm arrived in the Caribbean in the early decades of the eighteenth century. Towne’s 1726 testimony, quoted above, is among the earliest uses of the term ‘guinea worm’ and is also the earliest work to refer to the worm being most common along the Guinea coast between Anamaboe and Cormantyn (presumably Anamabo and Kormantse, both now in Ghana). This became another recurring description, as guinea worm became increasingly bound up with slavery [30, 31]. Guinea worm consequently arrived in the West Indies inside enslaved Africans, who often acquired the disease while imprisoned – Thomas Trotter, for instance, describes in detail (while attempting to prove a point about scurvy) how the waters of a ‘stagnant pool’ at the slave fort of Cape Coast Castle (now in Ghana) ‘had likewise the effect of producing the Guinea-worm among the Negroes first purchased, who had no signs of it till living on this water for some months’ [23]. Guinea worm, it must be noted, was not treated by Trotter as a serious problem, but merely as a demonstration of the unhealthiness of the water.
Eighteenth-century physicians knew that guinea worm was acquired from the waters of Guinea, and became convinced that dracunculiasis existed in the West Indies only as an imported disease. Stephen Freeman, for instance, wrote ‘I fancy it is not a disease [sic] of the West Indies; for all those I ever saw afflicted therewith, had brought it with them to the new world from Guinea’ [22]. This reinforced the idea that guinea worm was a particularly African disease, which was by this point common currency [13, 17, 32, 33]. And this reinforced the notion that it was not a serious problem for European medicine.
Ironically, it was during these decades that guinea worm gained a brief toehold in the Americas, from which it disappeared again in subsequent centuries, as described by Watts [4]. Hillary in 1766 reported from Barbados that he was ‘informed that there are some stagnating ponds in this Island, the washing in or drinking the Waters of which is subject to generate this Worm’ [13]. Colin Chisholm, meanwhile, in a 1795 footnote and an 1815 paper, described annual epidemics of guinea worm among enslaved labourers ‘on the estates of Edmund Thornton’ in Grenada, caused by contaminated wells ‘of which the whole gang drink’ [34, 35]. Filling in the wells and sinking new ones ended the epidemics. Transatlantic slavery brought guinea worm to the West Indies, but it was defined as a disease of Africans. Chisholm in 1795 presented himself as overturning an established doctrine:
‘Till within these few years, this disease was considered as peculiar to that part of the coast of Guinea contained between Cape Coast Castle and Acras, about ninety miles in extent: and it was believed that the slaves from the Gold Coast were alone subject to it, and always brought it with them to the West Indies, but never contracted it there. This however has been proved to be foundation; for the Creole-negroes are as subject to it as the Africans.’ [34]
But while dismissing the possibility that guinea worm was, as previous authors had believed, ‘peculiar to Africa’, he nevertheless framed it as a disease of ‘negroes’, rather than a threat to white health or a serious problem for European medicine. This, however, was soon to change.
BRITISH ENCOUNTERS WITH GUINEA WORM IN INDIA
The first decades of the nineteenth century saw an increasing interest in guinea worm, but not from the West Indian plantation doctors who had hitherto dominated dracunculiasis discourse. Instead, the papers which began to appear in the early nineteenth century English-language medical literature were mainly authored by military surgeons attached to Royal and East India Company (EIC) regiments based in India, who were beginning to encounter guinea worm through their duties. These were typically Scots who had graduated from Edinburgh and had few professional avenues available other than colonial service [36]. Journals such as the Edinburgh Physical and Medical Journal and the Transactions of the Medical and Physical Society of Calcutta, along with networks of private correspondence and barracks gossip, allowed British-Indian surgeons to learn, to circulate knowledge, and to speculate about the diseases they encountered – and these also provide information about how they interpreted diseases [37].
In 1855, Professor of Military Surgery George Ballinghall introduced guinea worm thus:
‘Of the several local affections which often prove a source of distress to individuals and of detriment to the service, upon foreign stations, there is perhaps none which holds a more prominent place than the troublesome affection produced by the Dracunculus or Guinea Worm.’ [38]
Guinea worm had become a significant military problem. And military surgeons were rising to the challenge: Ballinghall refers to ‘the numerous papers which have been written on this subject by medical officers in the service of Her Majesty or of the Honourable East India Company’ [38]. Articles on guinea worm published by India-based military surgeons such as James McGregor and Ninian Bruce (both of the Connaught 88th Regiment); James Anderson (Fort St. George); William Scot (Madras Artillery); John Milne (EIC medical service); and A. Duncan (Bombay) are an intermittent but regular feature of metropolitan (particularly Edinburgh) medical literature in the first decades of the nineteenth century [39-44]. Duncan even refers to the disease by an Indian name, Nharoo (Naru). Chisholm, meanwhile, inspired by the emerging debate and ‘contrariety of opinions’ about guinea worm’s causation in 1815 developed his 1795 notes into a detailed theory of guinea worm’s aetiology – one which emphasised geology, rather than race, as the most important factor in its transmission [35].
Sometimes guinea worm came back to Britain – Gilbert Burnett, for instance, reports treating a soldier’s wife named Anne Tennerson, recently returned from India, in London, while W.S. Oke records a seaman named John Stavely manifesting a worm acquired at Cape Coast Castle onboard a steamer bound for Southampton [45, 46]. Ballinghall even refers to specimens in Edinburgh University’s Anatomical Museum extracted from soldiers disembarking at Edinburgh or stationed in Canterbury [38].
The Transactions of the Medical and Physical Society of Bombay for 1859 include reports from surgeons based everywhere from Aden to Mount Abu, which depict dracunculiasis as a familiar problem. Statistics are often lacking but A.H. Leith of the European General Hospital recorded 11 cases in the year 1858-9, while Ruttonjee Hormusjee at Aden reported 84, and W.J. Stuart complained of 16 ‘of the finest and most healthy men of the [25th] regiment’ contracting dracunculiasis ‘and, although all recovered, it became necessary to permit many to return to their homes, as they were unfit for duty’ [47-49]. The description ‘tedious’ recurs frequently; these surgeons found guinea worm something of a frustration [47, 48].
INDIAN SPECIMENS IN BRITAIN AND THE DEVELOPMENT OF PARASITOLOGY
This frustration spawned a flow of knowledge and specimens back to London and Edinburgh, which brought guinea worm under the eye of the new science of zoology. Metropolitan scientists could now regularly read about guinea worm, while specimens from abroad accumulated in metropolitan museums such as Edinburgh University’s Anatomical Museum. There, they were studied by professional scientists – ‘new men’ of Victorian science – such as Thomas Spencer Cobbold, who examined the Museum’s guinea worms for his own research [36, 38]. Cobbold himself refers to examining Ballinghall’s ‘numerous fine specimens of Dracunculi’ [50]. The colonisation of India had made guinea worm into a military problem, but the specimens and knowledge provided by military surgeons trying to address this problem would further remake it into a zoological puzzle.
By the middle of the nineteenth century guinea worm no longer simply a disease. It had become an animal, an object of the emerging science of zoology. Zoologists such as Cobbold, Henry Bastian and Frederick Küchenmeister were busy putting guinea worm under the literal and figurative microscope to examine its anatomy and taxonomy. Physicians still referred to it as Dracunculus or guinea worm, but the zoologists, following the cues of Gmelin and Linnaeus, gave it a range of names, shifting the worm from taxon to taxon according to their present understandings. Küchenmeister preferred Filaria medinensis, Cobbold Dracunculus medinensis, while other authors claimed it a Gordius or a Furia, and the hybrid proposition of Filaria dracunculus also occurs [3, 50, 51].
The zoologists developed a visual and microscopical language for guinea worm, creating beautiful illustrations of the anatomical peculiarities of the worm, which would form the basis for the visual language of tropical medicine [50, 52]. Intestinal worms had been visualised in print since the eighteenth century, but guinea worm only with the advent of zoology [21]. Its anatomical structure, particularly the enormous uterus of the females, and the seeming absence of any males, was puzzled over, as the zoologists, aided by the availability of specimens from India, painstakingly defined guinea worm as a viviparous Filariid nematode with a long body, monstrous uterus, lack of anus, papillated head, white colouration and parasitic mode of life [50, 51]. Guinea worm was again a wonder, but this time due to its exotic (reproductive) anatomy. And it was a specifically zoological wonder: by 1866 Bastian could consider it in terms of similarity and difference to other Nematoids, and by 1880 the worm was so well-characterised that it could become, as in the works of Francis Maitland Balfour, a model organism for the embryonic science of embryology [53, 54]. By the 1870s, guinea worm featured in manuals and textbooks of zoology [55-57]. All this was facilitated by the ferrying of worms to the museums of Europe inside soldiers and the research of military surgeons such as Ballinghall.
GUINEA WORM RESEARCH IN GERMANY AND SAMARKAND
Nor was the influence of India was confined to the Anglosphere. The German zoological tradition which Farley claims dominated nineteenth-century parasitology was also indebted to British-Indian medicine, with influential German parasitologists such as Frederick Küchenmeister and Rudolf Leuckart drawing from British-Indian research on guinea worm – and being cited by British zoologists in turn [3, 50, 58, 59]. Indeed, it was a Russian parasitologist, Alexei Fedchenko, who discovered the role of cyclops as intermediate host of guinea worm.
‘Intermediate host’ is itself a zoological concept, and Cobbold claims that Fedchenko was put on the path of his discovery by Leuckart [60]. Leuckart had established that cyclops was the intermediate host of the worm Cucullanus, and it was therefore a zoological analogy to a related parasite which infected fish that led Fedchenko to consider whether guinea worm had an intermediate host [60]. Unlike the military surgeons who had previously researched guinea worm, Fedchenko approached the problem zoologically, assembling candidate intermediate hosts and housing them in an aquarium in his makeshift laboratory in Samarkand with guinea worm larvae [61]. An unnamed ‘native doctor, a specialist in extracting guinea worms’ (a mirimakason) provided Fedchenko with extracted adult female worms, from which he acquired guinea worm larvae, again reflecting that Fedchenko approached the problem as a zoologist, rather than a physician [62]. He viewed the worm not as a disease, but as an animal that that existed in interaction with other animals.
Fedchenko was able to find the cyclops because he approached guinea worm zoologically. But he was only able to recognise the ‘familiar-looking embryos of the guinea worm’ inside the cyclops because of the microscopical work done on Indian specimens by British scientists such as Cobbold, H.J. Carter (whom Fedchenko cited repeatedly) and George Busk [63, 64]. Military surgery fed zoology. Furthermore, Fedchenko implies he was only able to travel to Samarkand because of Russia’s recent conquest of Turkestan [61]. Military expansion facilitated zoological research in both the Russian and British Empires.
GUINEA WORM AND TROPICAL MEDICINE
Fedchenko’s discovery fed into the emerging discipline of tropical medicine, which was beginning to take shape at the end of the Nineteenth century, though via an indirect route. Fedchenko’s research was often cited in subsequent English-language literature on guinea worm, but his original paper, written in Russian and published in Moscow, was not. Fedchenko’s influence was mediated partly through Cobbold, whom Fedchenko had visited in 1873, but mostly via Leuckart [60]. Worboys has noted the friendship of Tropical Medicine’s founding father Patrick Manson with Cobbold – but when discussing guinea worm, Manson predominantly cited Leuckart [65, 66]. Manson also appropriated the visual language of zoology, copying Leuckart’s illustrations of guinea worm – which are themselves copied from Fedchenko (Figure 1). Manson’s own drawings similarly show a clear stylistic debt to Cobbold’s zoology (Figure 2). Despite their differing epistemological frameworks, knowledge circulated between zoology and medicine; zoology, itself fed by military surgery, fed the new tropical medicine.
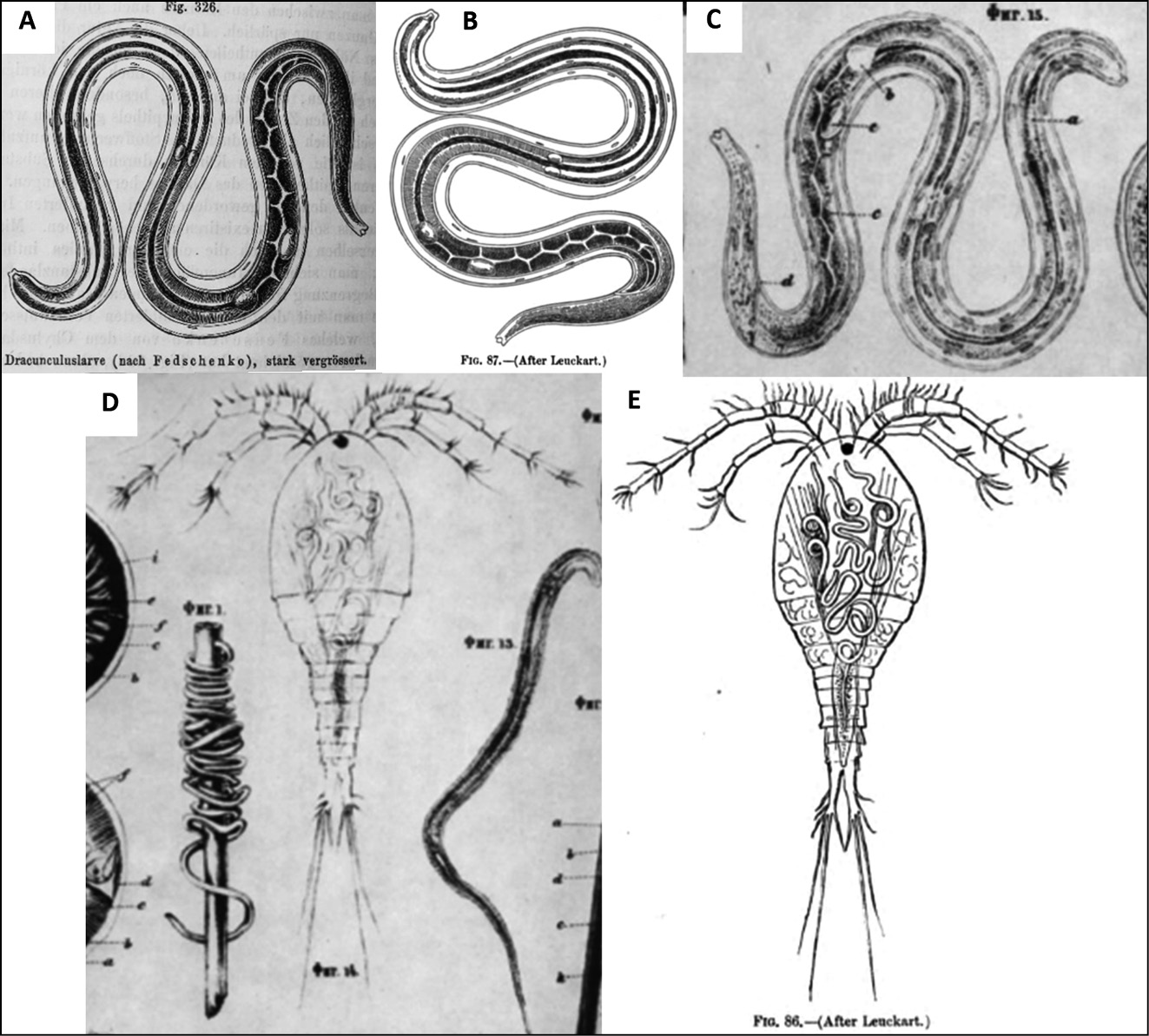
Figure 1 - Diagrams of guinea worm larvae, by Leuckart (A), Manson (B), and Fedchenko (C); and infected cyclops, by Fedchenko (D) and Manson (E).
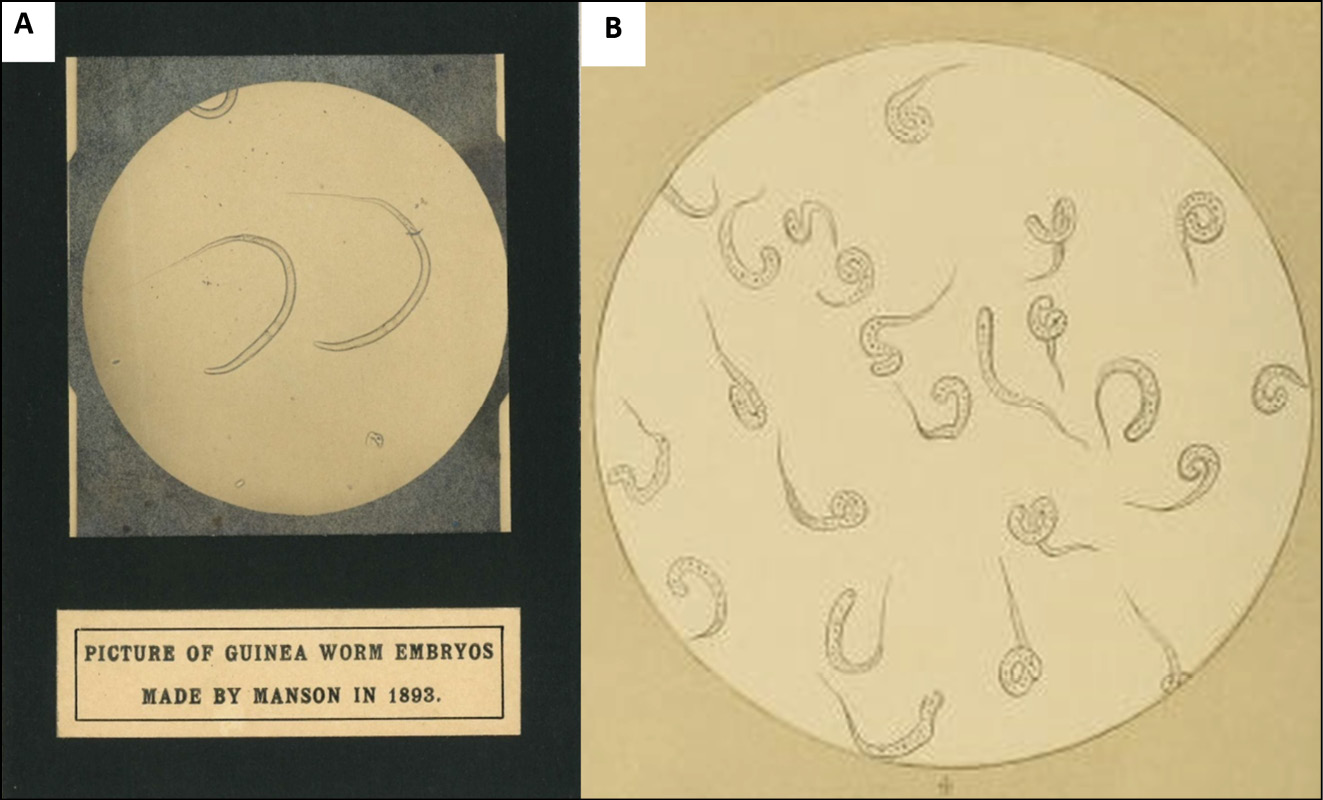
Figure 2 - Images of guinea worm larvae by Manson (A; Courtesy, London School of Hygiene & Tropical Medicine, LAORS, Archive Service) and Cobbold (B).
By 1905, when Robert Leiper was travelling across the British imperial peripheries of Africa to learn about guinea worm, as Fedchenko had travelled to the Russian imperial periphery of Samarkand some thirty years earlier, he did so as a student of tropical medicine rather than zoology [67]. But his work was grounded in zoology, and a 1910 letter sent by him to Ronald Ross shows a considerable interest at the London School of Hygiene and Tropical Medicine in the discoveries of Leuckart and Fedchenko [68]. And Leiper, discovering the role of stomach acid in dissolving the cyclops and allowing the guinea worm larvae to escape the stomach, is credited with solving the final puzzle in the lifecycle of guinea worm [5, 69].
GUINEA WORM ERADICATION IN BUKHARA
This was not the end of research into guinea worm. The energetic and ultimately successful efforts of Leonid Isaev and the Bukhara Tropical Institute to eradicate the disease from Bukhara (called rishta in Turkestan, and by then entirely an object of tropical medicine) between 1923 and 1931 also generated a small corpus of research, which deserves the attention of a skilled historian fluent in Russian and Uzbek [62, 70-72]. But amid the turmoil of the Russian Revolution – Bukhara’s guinea worm eradication programme outlived both of its republics – this knowledge, unlike Fedchenko’s, does not seem to have managed to travel to Europe, where interest in guinea worm was waning [73]. In some respects guinea worm research was a victim of its own success. Not only did Cobbold, Fedchenko, Leiper and the rest leave precious few puzzles for future scientists to solve, but, as in Bukhara, practical research into effective control methods could result in the supply of specimens – which, as the case of British-Indian medical and zoological research into guinea worm demonstrates, were crucial and mobile sources of knowledge – drying up.
CONCLUSIONS
There were, from 1688 to 1931, several transformations of guinea worm, from a curiosity of far-off lands, to an African disease, to a British imperial military problem, to a zoological puzzle, before it settled within the discipline of tropical medicine as a tropical disease (Table 1). Dracunculiasis demonstrates the long history of the antecedents of tropical medicine, and how tropical medicine grew out of not only the naval, colonial and British-Indian medical traditions, but also from zoology. Military medicine provided parasitology not only with knowledge and specimens, but also with an organism – guinea worm – that provided both a source of puzzles and a visible reference point for the mostly microscopic nematodes [74].
Table 1 - Changing perceptions of guinea worm in English-language texts over time.
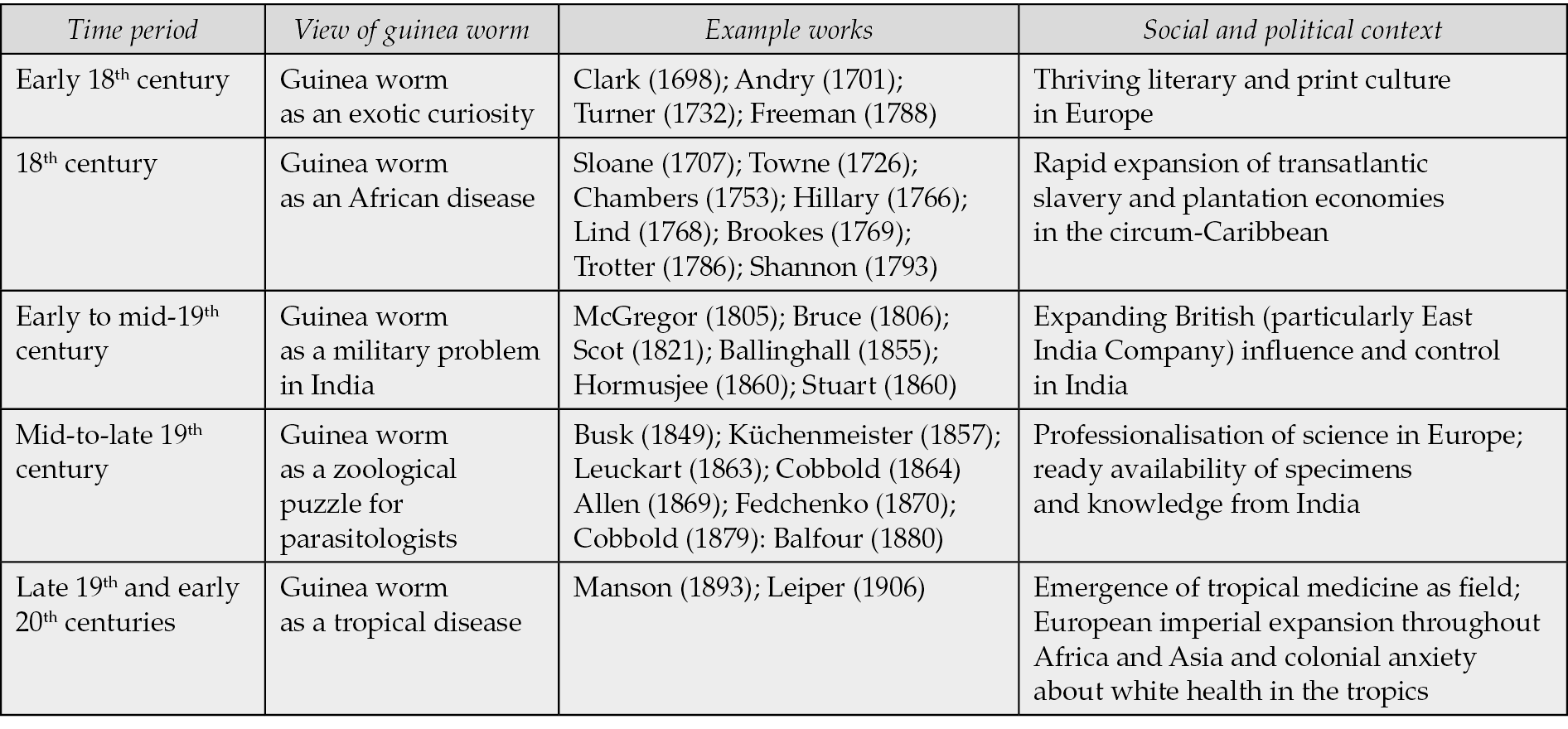
Worboys shows that the precursor disciplines to tropical medicine were British naval medicine, colonial medicine and British-Indian medicine, and that these, alongside tropical medicine itself, were shaped by military and imperial need [65]. Changing attitudes towards guinea worm support this, and also underline that guinea worm was problematised only when it affected soldiers. The importance of Empire and colonisation in shaping the natural sciences has long been noted by historians of science, but guinea worm shows how colonial military encounters with a parasite facilitated flows of knowledge and specimens from imperial periphery to metropolitan centre, shaping the development of the civilian science of zoology [75-77]. Both Worboys and Haynes note the influence of zoologists such as Cobbold on the subsequent development of tropical medicine, but guinea worm shows Cobbold himself benefiting from military knowledge and specimens [36, 65].
The history of guinea worm science, furthermore, is global, encompassing locations the Caribbean, West Africa, India, and Central Asia (Figure 3). Crucial research was carried out not only in Edinburgh and Leipzig, but also in Samarkand and Calcutta (Kolkata), as knowledge and specimens circulated around the globe.
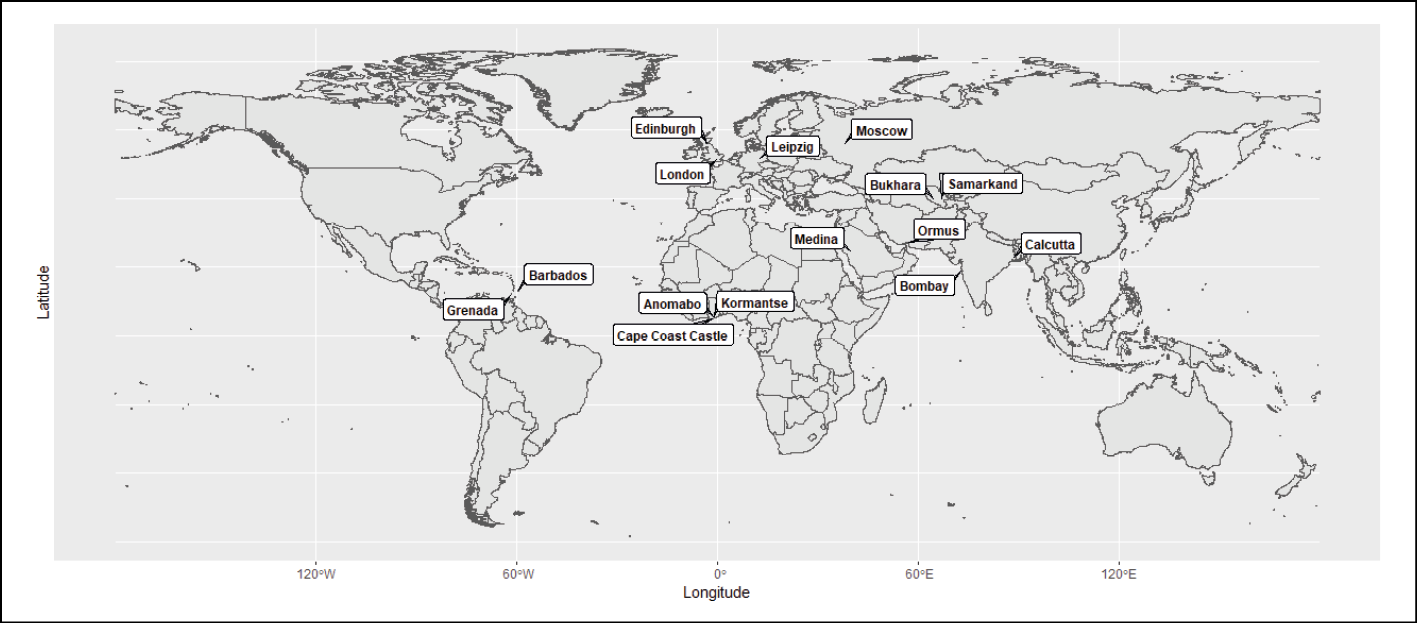
Figure 3 - Significant locations in the history of guinea worm referred to in this article.
Conflicts of interest
None to declare:
Funding
This research was self-funded.
Acknowledgements
This paper is adapted from the first chapter of my MSc thesis in the History of Science, Medicine and Technology at the University of Oxford. I am deeply indebted to the help of my then supervisor Professor Erica Charters, and all the hard work she put in to supporting me to undertake this research. I would also like to thank Serena Turton-Hughes for her insightful feedback on the early drafts of this paper!
REFERENCES
[1] Despommier DD. People, Parasites and Plowshares. Columbia University Press, New York. 2013.
[2] Edungbola LE. Dracunculiasis (Guinea Worm Disease) Eradication in Nigeria: An Eyewitness Account. Elsevier, Oxford; 2019.
[3] Küchenmeister F. Animal and Vegetable Parasites of the Human Body (trans. E. Lankester). Sydenham society, London; 1857.
[4] Watts S. Dracunculiasis in the Caribbean and South America. Medical History. 2000; 45(1): 227-250.
[5] Tayeh A, Cairncross S, Cox FEG. Guinea Worm: From Robert Leiper to Eradication. Parasitology. 2017; 144(1): 1643-1648.
[6] Biswas G, Sankara DP, Agua-Agum J, Miaga A. Dracunculiasis (guinea worm disease): Eradication without a drug or a vaccine. Philosophical Transactions of the Royal Society B. 2013; 368(1623): 1-13.
[7] Simonetti O, Zerbato V, Bella SD, Luzatti R, Cavalli F. Dracunculiasis over the centuries: the history of a parasite unfamiliar to the West. Infez Med. 2023; 31(2): 257-264.
[8] Cairncross S, Miller R, Zagaria N. Dracunculiasis (Guinea Worm Disease) and the Eradication Initiative. Clinical Microbiology Reviews. 2002; 15(2): 223-246.
[9] Clark R. Vermiculars Destroyed... London. 1698.
[10] Greenblatt S. Marvelous Possessions. Oxford University Press, Oxford. 1991.
[11] Davies S. Renaissance Ethnography and the Invention of the Human. Cambridge University Press, Cambridge. 2016.
[12] Freind J. History of Physick. 3rd Edition London. 1725.
[13] Hillary W. Observations on the changes of the air and the concomitant epidemical diseases, in the island of Barbadoes. To which is added A treatise on the putrid bilious fever, commonly called the yellow fever.... 1766.
[14] Browne J. A natural and medicinal history of worms. London. 1721.
[15] Kaempfer E. Amoenitatum exoticarum politico-physico-medicarum fasciculi... Lemgoviae. 1712.
[16] Kaempfer E. History of Japan (trans. J.G. Scheuchzer). London. 1707.
[17] Sloane H. A voyage to the islands Madera, Barbados... London. 1707.
[18] Towne R. A treatise of the diseases most frequent in the West-Indies. London. 1726.
[19] Turner D. The Art of Surgery. 4th Edition. London. 1732.
[20] Mead R. Medical Precepts and cautions... London. 1751.
[21] Andry N. An Account of the Breeding of Worms in Human Bodies. 1701.
[22] Freeman S. The ladies’ friend and family phycial library... London. 1788.
[23] Trotter T. Observations on the scurvy... Edinburgh. 1786.
[24] McNeill JR. Mosquito empires: ecology and war in the Greater Caribbean, 1620-1914. Cambridge University Press, Cambridge. 2010.
[25] Darwin E. Zoonomia... 2nd Edition. London. 1796.
[26] Nickolls RB. Letter to the treasurer... London. 1788.
[27] Grainger J. The sugar-Cane: A Poem in Four Books. London. 1764.
[28] Desen. E, Leem Z-Y, Hill A, Notz Q, Patel JJ, Stoppe C. History of scurvy and use of vitamin C in critical illness: A narrative review. Nutr Clin Pract. 2023; 38.
[29] Lind J. An essay on diseases incidental to Europeans in hot climates With the method of preventing their fatal consequences... London. 1768.
[30] Anon. The modern dictionary of arts and sciences. London. 1774.
[31] Chambers E. A supplement to Mr. Chambers’s Cyclopaedia. London. 1753.
[32] Brookes R. An exlaination of the terms of art... London. 1769.
[33] Shannon R. Practical observations on the operation and effects of certain medicines. London. 1793.
[34] Chisholm C. An essay on the malignant pestilential fever introduced into the West Indian Islands from Boullam. London. 1795.
[35] Chisholm C. On the Malis Dracunculus. Edinburgh Medical and Surgical Journal. 1815; 11(42): 145-164.
[36] Haynes DM. Imperial Medicine: Patrick Manson and the Conquest of Tropical Disease. University of Pensylvania Press, Philadelphia. 2001.
[37] Harrison M. Climates and Constitutions. Oxford University Press, Oxford. 1999.
[38] Ballinghall G. Outlines of Military Surgery. Adam and Charles Black, Edinburgh. 1855.
[39] McGregor J. On the Diseases of the 88th Regiment in Bombay. Edinburgh Medical and Surgical Journal. 1805; 1(3): 266-289.
[40] Bruce N. Remarks on the Dracunculus or Guinea Worm. Edinburgh Medical and Surgical Journal. 1806; 2(6): 145-150.
[41] Anderson J, Dubois. History of the Guinea Worm. Edinburgh Medical and Surgical Journal. 1806; 2(7).
[42] Scot W. Remarks on the Dracunculus or Guinea Worm. Edinburgh Medical and Surgical Journal. 1821; 17(66): 96-105.
[43] Grant R, Milne J. Extracts from a Correspondance on the Filaria Medinensis. Edinburgh Medical and Surgical Journal. 1831; 35(106): 112-118.
[44] Duncan A. Observations on Dracunculus. Transactions of the Medical and Physical Society of Calcutta. 1835; 7(2): 273-282.
[45] Burnett GT. Case of Dracunculus, or Filaria Medinensis. London Medical and Physical Journal. 1830; 9(52): 285-291.
[46] Oke WS. Case of Filaria Medinenis, or Guinea Worm. Provincial Medical Journal. 1843; 6(152): 446-447.
[47] Leith AH. Annual Report of the European General Hospital for the Year 1858-59. Transactions of the Medical and Physical Society of Bombay. 1860; V(1): 89-105.
[48] Hormusjee R. Annual Report of the Sick of the Engineer Department at Aden for the Year 1856-7. Transactions of the Medical and Physical Society of Bombay. 1860; V(1): 51-66.
[49] Stuart WJ. Annual Report of the 25th Regiment N.L.I. for the Year 1858-59. Transactions of the Medical and Physical Society of Bombay. 1860; V(1): 10-43.
[50] Cobbold TS. Entozoa: An Introduction to the Study of Helminthology, with Reference, More Particularly, to the Internal Parasites of Man. Groombridge and Sons, London. 1864.
[51] Diesing KM. Systema Helminthum. W. Braumüller, Vindobonae. 1851.
[52] Carter HJ. On Dracunculus and microscopic Filaridae in the island of Bombay. Annals and Magzine of Natural History. 1859; 4(20): 98-116.
[53] Bastian HC. On the Anatomy and Physiology of the Nematoids. Philosophical Transactions of the Royal Society. 1866; 156(1): 545-639.
[54] Balfour FM. A Treatise on comparative embryology. MacMillian and Co., London. 1880.
[55] Nicholson HA. Manual of Zoology. Blackwood, Edinburgh. 1870.
[56] Allen H. Outlines of comparative anatomy and medical zoology. J.B. Lippincott and Co., Philadelphia. 1869.
[57] Boas JEV. Text-book of Zoology. Sampson Low, London. 1896.
[58] Farley J. The Spontaneous Generation Controversy. Journal of the History of Biology. 1972; 5(1): 95-125.
[59] Lueckart R. The Parasites of Man and the diseases which proceed from them. A text book for students and practitioners (trans. W.E. Hoyle). Young J. Pentland, Edinburgh. 1886.
[60] Cobbold TS. Parasites : a treatise on the entozoa of man and animals, including some account of the ectozoa. J. & A. Churchill, London. 1879.
[61] Fedchenko AP. Concerning the Structure and Reproduction of the Guinea Worm Proceedings of the Imperial Society of the Friends of Natural Sciences. 1870; 8: Reprinted and trans. (by E. Naust) in American Journal of Tropical Medicine and Hygiene. 1971; 20(4): 511-523.
[62] Uzbekistan Ministry of Health, Dracunculiasis Eradication in Uzbekistan: Country Report. WHO Archive. 1998; WHO/CDS/CEE/DRA99.9.
[63] Carter HJ. Observations on Dracunculus in the Island of Bombay. Annals and Magzine of Natural History. 1858; 1(6): 410-414.
[64] Busk G. Observations on the Structure and Nature of the Filaria medinensis. Transactions of the Microscopical Society of London. 1849; 2(1): 65-76.
[65] Worboys M. The Emergence of Tropical Medicine. In: Lemaine G, MacLeod R, Mulkay M, Weingart P, editors. Perspectives on the Emergence of Scientific Disciplines.Masion de Sciences de L’Homme, Chicago. 1976.
[66] Manson P. Diseases of the Skin. In: Davidson A, editor. Hygiene and Diseases of Warm Climates. Young J. Pentland, Edinburgh. 1893.
[67] Leiper R. Postcards sent by R. Leiper to LSHTM from various locations across Africa. London School of Hygiene and Tropical Medicine Archive. 1905-1907; Leiper/02/02/01 through Leiper/02/02/35.
[68] Lieper R. Letter from R. Leiper to R. Ross (21 Jan 1910) regarding the development of D. medinensis and the role of Cyclops as the intermediate host. London School of Hygiene and Tropical Medicine Archive. 1910; Ross/138/01/31.
[69] Leiper RT. The influence of Acid on Guinea Worm Larvae. British Medical Journal. 1906; 1(2349): 19-20.
[70] Isaev LM. A simple method for mass extermination of crustaceans for larvae of parasitic worms. Meditsinskaia parazitologiia i parazitarnye bolezni. 1934; III(3): 212-240.
[71] Kadyrov AA, Madakhanov AS. Pervyı̆ meditsinskiı̆ institut Uzbekistana. Sovetskoe zdravookhranenie. 1980; 1980(6): 57-58.
[72] Litvinov SK. How the USSR rid itself of dracunculiasis. World Health Forum. 1991; 12(2): 217-219.
[73] Khalid A. Making Uzbekistan: Nation, Empire and Revolution in the Early USSR. Cornell University Press, London. 2016.
[74] Kuhn TS. The Structure of Scientific Revolutions. Chicago University Press, London. 2012.
[75] Parish SS. American Curiosity: Cultures of Natural History in the Colonial British Atlantic World. University of North Carolina Press, Chapel Hill. 2006.
[76] Barrera-Osorio A. Experiencing Nature: The Spanish American Empire and the early Scientific Revolution. University of Texas Press, Austin. 2006.
[77] McClellan JE, Regourd F. The Colonial Machine: French Science and Overseas Expansion in the Old Regime. Brepols, Tournhout. 2012.