Le Infezioni in Medicina, n. 1, 99-102, 2024
doi: 10.53854/liim-3201-13
CASE REPORTS
An unusual case of Brucella melitensis-related wound infection
Ozge Alkan Bilik1, Fatma Meral Ince 2, Nida Ozcan3, Zeynep Ayaydin4
1Medical Microbiology Laboratory, Selahaddin Eyyubi State Hospital, Diyarbakir, Turkey;
2Infectious Diseases and Clinical Microbiology, Selahaddin Eyyubi State Hospital, Diyarbakir, Turkey;
3Dept. of Medical Microbiology , Dicle University Faculty of Medicine, Diyarbakir, Turkey;
4Medical Microbiology Laboratory, Gazi Yas argil Training and Research Hospital, Diyarbakir, Turkey.
argil Training and Research Hospital, Diyarbakir, Turkey.
Received 6 December 2023, accepted 8 February 2024
Corresponding author
Nida Ozcan,
E-mail: nidaok@yahoo.com
SummaRY
Background: Brucellosis is an anthropo-zoonotic infectious disease caused by various Brucella species. It is usually transmitted through contact with infected animals or consumption of contaminated animal products. Brucellosis most commonly affects the musculoskeletal and reticuloendothelial system with additional involvement observed in gastrointestinal system, urinary tract, reproductive system, central nervous system, and cardiovascular system. Skin involvement is extremely rare in brucellosis. Here, we report a rare case of Brucella melitensis infection developing in a back wound following a lumbar disc herniation surgery over 14 years ago.
Case: A 34-year-old male patient, who had a herniated disc surgery 14 years ago, was admitted to the hospital with complaints of joint pain, sweating and discharge at the surgery site. Wound culture revealed the presence of Gram negative cocobacilli which was identified as Brucella melitensis. The subsequent diagnostic tests, including the Rose-Bengal and Brucella Capture test positivity at a titer of 1/320 confirmed the diagnosis.
The patient received six weeks of doxycycline (200 mg/day, orally) and rifampin (600 mg/day orally) treatment, accompanied by wound care procedures. Daily cleaning, sterile dressing, and wound debridement were employed. Following treatment, the patient’s condition improved, and wound discharge ceased. Continuous monitoring showed no signs of relapse, achieving complete remission.
Conclusion: Brucella spp. should be considered as a potential cause of wound infections developing after surgery or trauma in brucellosis-endemic areas. This report also emphasizes the importance of promptly determining the cause of infection before initiating antibiotic treatment.
Keywords: Brucella melitensis, Brucellosis, Wound infection, Wound care.
INTRODUCTION
Brucella genus, an intracellular Gram-negative coccobacillus, predominantly utilizes sheep and goats as reservoirs, with the species B. melitensis posing the highest risk of human infection. Brucellosis, among the most prevalent zoonotic diseases globally and notably endemic in our region, is often transmitted to humans through the consumption of unpasteurized dairy products of infected animals [1, 2]. The clinical presentation of brucellosis varies widely, manifesting as a non-specific febrile illness that can affect virtually any system [3]. Remarkably, brucellosis is associated with atypical side effects and unusual clinical presentations, as documented in various investigations [4, 5]. The reported incidence of skin involvement in brucellosis ranges from 0.4% to 17.0%. While wound infections are typically attributed to Staphylococcus aureus and Streptococcus pyogenes, Brucella melitensis is a rare causative agent in such cases [6-8].
This case report examines a 34 years old patient who initially presented with a wound infection. Subsequent analysis of the wound culture revealed the growth of Brucella melitensis, leading to the diagnosis of brucellosis.
CASE PRESENTATION
A 34-year-old male patient, employed as a livestock farmer, underwent lumbar disc herniation surgery approximately 14 years before. Recently, he presented with a wound infection characterized by purulent discharge in the surgical area that has persisted for 20 days. The patient did not benefit from various antibiotic treatments administered at different centers, including amoxicillin-clavulanate and topical fusidic acid. The patient was admitted to infectious diseases outpatient clinic with complaints of back pain, and discharge in the operation area (Figure 1). The patient also stated that he sometimes complained of fever and sweats. A swab sample was collected from the purulent discharge for culture, and empiric treatment with ciprofloxacin (500 mg/12 h) and sodium fusidate (topically twice daily) was initiated. The sample was inoculated onto sheep blood agar (SBA), Eosin Methylen Blue (EMB) agar, and chocolate agar media (all from RTA, Turkey) and incubated at 35±2ºC for 72 hours. On the third day of incubation, small colonies grew on SBA and chocolate agar media. The colonies exhibited positive results in catalase, oxidase, and urease tests. Gram staining revealed the presence of small Gram-negative coccobacilli. The automated Vitek 2 Compact system (BioMerieux, France) identified the growing bacteria as Brucella melitensis. The patient was recalled to the outpatient clinic and a venous blood sample was taken for serological tests. It was revealed that the patient had not experienced brucellosis symptoms previously, but had been suffering from joint pain for the last 1.5 months and night sweats in recent days. Agglutination was observed in the Rose-Bengal test (Biomedica-Diagnostic, Canada). The Brucella Capture test revealed a positive agglutination at a titer of 1/320 using the BrucellaCAPT test (Vircell, Spain). A contrast-enhanced lumbar MRI (magnetic resonance imaging) revealed no evidence of spondylodiscitis. After being diagnosed with brucellosis, the patient’s existing antibiotic treatment was discontinued. Subsequently, the patient commenced a regimen of doxycycline 100 mg/12 h and rifampicin 600 mg/day. Concurrently, wound debridement and daily changes of sterile, non-adherent dressings were administered. The patient exhibited clinical improvement after six weeks of brucellosis treatment, and drainage at the wound site ceased (Figure 2). Throughout the treatment course, the patient was closely monitored, showing no signs of relapse, and achieving complete remission.
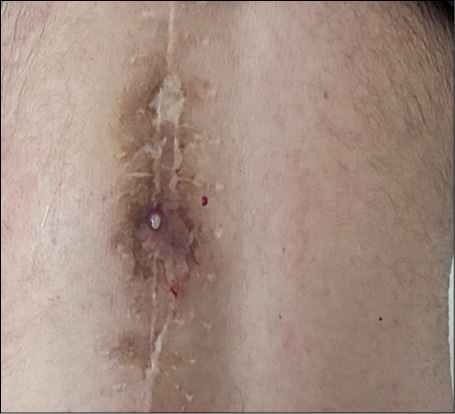
Figure 1 - The wound with purulent discharge in the surgical area.

Figure 2 - The wound after medical treatment.
DISCUSSION
Brucellosis, a systemic infection prevalent worldwide, is also endemic in Turkey [9]. It has the potential to affect any organ or tissue in the human body. Notably, skin and soft tissue involvement represent unusual features in brucellosis [10]. Consequently, there is a paucity of studies examining cutaneous lesions associated with brucellosis.
The patient’s surgical history and the presence of a wound at the surgical site suggested the involvement of pyogenic bacteria which were the most common infectious organisms associated with abscess development. This typically includes bacteria such as Staphylococci, Streptococcus pyogenes, or, less commonly, atypical Mycobacteria species [8, 11]. Due to its non-specific symptoms, brucellosis patients may be mistakenly diagnosed as having other bacterial infections [7].
It is widely recognized that Brucella species can enter the body through cuts or abrasions in the skin, particularly among livestock farmers and those working in abattoirs [3]. This direct inoculation and hematogenous invasion of skin or soft tissues can lead to various skin infections [7]. While skin manifestations of brucellosis are uncommon, they have been documented in the early stages of the illness [3]. Given the patient’s occupation, it is plausible that the infection was contracted through the consumption of raw milk or close contact with infected animal products.
Similar to our case, in Iran, Nejadeh et al. reported a rare case of Brucella melitensis wound infection. The patient had an infected wound on his left leg as a result of a traffic accident 13 years before. Remarkably, the man was engaged in animal husbandry in the town of Pishva, surrounded by agricultural areas in Tehran province, and frequently consumed raw dairy products [12]. Another case report from Iran revealed two ulcerative abscesses due to Brucella abortus in a 40-year-old shepherd’s lower left leg [13]. A rare case of a cutaneous abscess due to Brucella melitensis on the left foot of a 3-year-old girl was reported by Resendiz-Sanchez from Mexico. The authors hypothesized that the original skin lesion must have been contaminated with infected animal material because the child had been drinking unpasteurized milk since age 1[14]. Regarding our patient, we have no definitive evidence that the wound was the result of direct inoculation with bacteria or drinking contaminated unpasteurized milk. Therefore, in brucellosis-endemic regions, Brucella species should be considered causative agents in wound infections developing after trauma or surgery.
Given its vague symptoms and the requirement for advanced culture methods, diagnosing brucellosis can be challenging. While blood culture remains the gold standard, serological testing are also known to be highly beneficial in the diagnostic process [15]. The Rose Bengal test is often used as a screening tool, and positive results are subsequently confirmed by serum agglutination testing [16]. In the present case, the positivity of both the Rose Bengal test and the Brucellacapt agglutination tests supported the diagnosis. Although dermatological findings lack specificity in the context of brucellosis, diagnostic utility can be derived from culture and serological laboratory findings.
To mitigate the risk of future illness complications, it is imperative to secure an early diagnosis and initiate appropriate treatment promptly. The management of wound infections induced by brucellosis is contingent upon rigorous wound care practices. Furthermore, it is crucial to consistently cleanse and dress wounds to prevent the accumulation of pus and other infectious materials [17]. The wound care of the present case was performed appropriately.
CONCLUSIONS
It is crucial to extend the incubation period in wound culture evaluations to at least three days to detect fastidious bacteria effectively. It should be noted that fastidious microorganisms, such as Brucella species may infrequently be implicated in wound infections. Brucella related infections should be considered in patients who do not respond to antibiotic therapy and show no growth in previous cultures particularly in brusellosis-endemic areas.
In cases of brucellosis-related wound infections, standard brucellosis treatment accompanied by wound debridement and daily sterile dressing are recommmended.
This case report presents an atypical manifestation of wound infection caused by Brucella melitensis and highlights the important role of wound culture in the diagnosis of the disease. Early detection, timely diagnosis, and appropriate wound care can mitigate complications and expedite recovery.
Conflicts of interest
None
Funding
None
Acknowledgements
A written consent was obtained from the patient.
REFERENCES
[1] Pappas G, Akritidis N, Bosilkovski M, Tsianos E. Brucellosis. N Engl J Med. 2005; 352(22): 2325-2236. doi: 10.1056/NEJMra050570.
[2] Buzgan T, Karahocagil MK, Irmak H, et al. Clinical manifestations and complications in 1028 cases of brucellosis: a retrospective evaluation and review of the literature. Int J Infect Dis. 2010; 14(6): e469-e478. doi: 10.1016/j.ijid.2009.06.031.
[3] Kudvah AJN. Cutaneous and Soft Tissue Brucellosis, In Madkour’s Brucellosis (Madkour MM. Ed). Springer Berlin, Heidelberg; 2012: 193-200.
[4] Yilmaz M, Arslan F, Başkan Ö, Mert A. Splenic abscess due to brucellosis: a case report and a review of the literature. Int J Infect Dis. 2014; 20: 68-70. doi: 10.1016/j.ijid.2013.11.010.
[5] Tekin R, Ceylan Cevik F, Ceylan Tekin R, Cevik R. Brucellosis as a primary cause of tenosynovitis of the extensor muscle of the arm. Infez Med. 2015; 23(3): 257-260.
[6] Karaali Z, Baysal B, Poturoglu S, Kendir M. Cutaneous manifestations in Brucellosis. Indian J Dermatol. 2011; 56(3): 339. doi: 10.4103/0019-5154.82505.
[7] Korkmaz P, Kartal ED. Skin manifestations associated with brucellosis. EMJ Dermatol. 2016; 4(1): 119-125. doi: 10.33590/emjdermatol/10312753.
[8] Baron EJ, Miller JM, Weinstein MP. et al. A guide to utilization of the microbiology laboratory for diagnosis of infectious diseases: 2013 recommendations by the Infectious Diseases Society of America (IDSA) and the American Society for Microbiology (ASM). Clin Infect Dis. 2013; 57(4): e22-e121. doi: 10.1093/cid/cit278.
[9] Young EJ. Brucella Species, In: Principles and Practice of Infectious Diseases (Mandell, G.L., Bennett, J.E. and Dolin, R., Eds.,). 6th Edition, Churchill Livingstone, Philadelphia; 2005: 2669-2672.
[10] Berger TG, Guill MA, Goette DK. Cutaneous lesions in brucellosis. Arch Dermatol. 1981; 117(1): 40-42.
[11] Sarrou S, Skoulakis C, Hajiioannou J. et al. Brucella melitensis as causative agent for neck abscess in an endemic area. Balkan Med J. 2017; 34(1): 78-80. doi: 10.4274/balkanmedj.2015.1143.
[12] Nejadeh AH, Nejadeh S, Jamshidi ML. et al. Manifestation of Brucella infection post an accident: A case report. J Clin Images Med Case Rep. 2022; 3(11): 2138. doi:10.52768/2766-7820/2138.
[13] Shahabi Nejad N, Eftekhari N, Shahabi Nejad S. A Case of Multi-Ulcerative Abscess Due to Brucella abortus in Kerman, South East of Iran. Iran J Med Sci. 2018 Sep; 43(5): 546-549.
[14] Resendiz-Sánchez J, Contreras-Rodríguez A, López-Merino A, Bravo-Guzmán L, Valle-Valdez JG. Isolation of Brucella melitensis from an abscess on the left foot of a 3-year-old infant. J Med Microbiol. 2009; 58(Pt 2): 267-269. doi: 10.1099/jmm.0.004291-0.
[15] Franco MP, Mulder M, Gilman RH, Smits HL. Human brucellosis. Lancet Infect Dis. 2007; 7(12): 775-786. doi: 10.1016/S1473-3099(07)70286-4.
[16] Al Dahouk S, Tomaso H, Nöckler K, Neubauer H, Frangoulidis D. Laboratory-based diagnosis of brucellosis - a review of the literature. Part II: serological tests for brucellosis. Clin Lab. 2003; 49(11-12): 577-589.
[17] Selvaraj D, Viswanadha VP, Elango S. Wound dressings-a review. Biomedicine. 2015; 5(4): 22. doi: 10.7603/s40681-015-0022-9.