Le Infezioni in Medicina, n. 1, 104-108, 2022
doi: 10.53854/liim-3001-12
ORIGINAL ARTICLE
Epidemiology of respiratory virus before and during COVID-19 pandemic
Manuela Avolio1, Sergio Venturini2, Rita De Rosa1, Massimo Crapis2, Giancarlo Basaglia1
1Department of Microbiology, ASFO Santa Maria degli Angeli Hospital, Pordenone, Italy;
2Department of Infectious Diseases, ASFO Santa Maria degli Angeli Hospital, Pordenone, Italy
Article received 13 December, 2021, accepted 8 January 2022
Corresponding author
Manuela Avolio
E-mail: manuela.avolio@asfo.sanita.fvg.it
SummaRY
The COVID pandemic has forcefully turned the spotlight on the importance of the diagnosis of respiratory virus infections. Viruses have always been a frequent and common cause of respiratory tract infections. Rapid molecular diagnostics applied to the diagnostics of respiratory virus infections has revolutionized microbiology laboratories only a few years ago. Few studies illustrate the epidemiology of respiratory viruses, and fewer still those that have compared the pre-pandemic to the pandemic period. During the first year of the pandemic (2020-2021) it was clear to everyone to witness a sudden disappearance of the circulation of all the other respiratory viruses, especially those typically isolated during the winter time, such as RSV and Influenza virus. In our study we wanted to verify this phenomenon and to study the epidemiology of our local reality, analyzing three consecutive flu seasons (2018-2019, 2019-2020, 2020-2021). The results lead us to note that the prevalence of positivity to respiratory virus infections went from 49.8% (2018-2019) and 39% (2019-2020) to 13.4% (2020-2021). This decrease is at least partly attributable to the security measures adopted (social distancing and mask), but it certainly opens up new scenarios when the restriction measures will be terminated. We believe such studies can provide real-world evidence of the effectiveness of public health interventions implemented during current and future pandemics.
Keywords: respiratory virus epidemiology, flu-season, COVID-19 pandemic.
INTRODUCTION
In December 2019, Severe Acute Respiratory Syndrome coronavirus 2 (SARS-CoV-2) was first identified in clusters of pneumonia cases of unknown origin in Wuhan, China [1]. The SARS-CoV-2 spread rate has increased exponentially worldwide. The Italian government confirmed the country’s first cases of the disease on 30 January 2020, when the virus was detected in two Chinese tourists visiting Italy [2]. The first SARS-CoV-2 positive case in Pordenone (North East Italy) was diagnosed on 7 March 2020. On 9 March 2020, the Italian government imposed a national lockdown thus several public health measures were adopted as cancellation of public events, stay-at-home, school closures, workplace closures, international travel restrictions mask-wearing recommendation, mandatory use of masks in enclosed public spaces. The World Health Organization declared the global outbreak of COVID-19 as a pandemic on 11 March 2020 [3].
Before COVID-19 pandemic, Acute Respiratory Infections (ARI) have always been a major cause of morbidity and mortality. Although it is estimated that the viral causative agent is involved in up to 80% of cases, most of these agents have never been investigated routinely and specifically so far. Influenza viruses are one of the major etiological agents of ARI. However, many other respiratory viruses for which insufficient epidemiological information has been available to date can also cause ARI, in both pediatric and adult populations [4-6]. Many respiratory viruses cause high hospitalization rates and sometimes improper use of antibiotic therapy if not correctly diagnosed [6].
Until about ten years ago, the diagnosis of the viral causative agent in ARI was the prerogative of a few laboratories, but in the last decade the rapid molecular diagnostics applied to the respiratory virus infections has revolutionized the diagnostic approach of the microbiology laboratories [6, 7]. However, few studies illustrate the epidemiology of respiratory viruses, and fewer still those that have compared the pre-pandemic to the pandemic period [8].
In light of the pandemic we are going through, we thought the following two questions: what seasonality of the respiratory viruses other Sars-CoV2 circulating before the pandemic? During pandemic, how much have social restriction measures and the use of safety devices affected the circulation of all respiratory virus? To answer to these questions, we aimed to evaluate in our local contest the impact, in hospitalized patients, of not SARS-CoV-2 respiratory virus in 2020-2021 (pandemic time), by comparing their trends in detection with 2018-2019 period (pre-pandemic time).
MATERIALS AND METHODS
Overall, 6206 clinical respiratory specimens (nasopharyngeal swabs or bronchoalveolar lavage) collected between May 2018 and April 2021 from adult and paediatric hospitalized patients with symptoms of ARI, were tested by multiplex real-time PCR Allplex respiratory panel (All16, Seegene, Seoul, Republic of Korea) detecting: Influenza virus A (FluA) and B (FluB), Adenovirus (AdV), Coronavirus (229E, NL63, OC43) (CoV), 1/2/3/4 human Bocavirus (HBoV), human Enterovirus (HEV), human Metapneumovirus (MPV), human Rhinovirus A/B/C (HRV), 1/2/3/4 Parainfluenza virus (PIV), Respiratory Syncytial Virus A (RSVA) and B (RSVB).
We divided the entire observed period into three consecutive flu seasons: May 2018-April 2019, May 2019 - April 2020 and May 2020-April 2021.
RESULTS
Out of 6206 specimens analyzed between May 2018 and April 2021, 2198, 3211 and 797 were analyzed in 2018-2019, 2019-2020 and 2020-2021 respectively.
Out of 6206 total specimens, 2452 (39.5%) resulted positives. Table 1 shows the population examined (adults and children hospitalized for flu-like symptoms, and positive for any respiratory virus), and demographic characteristics, units, and the median age of greatest circulation, for each viral subtype detected, are reported.
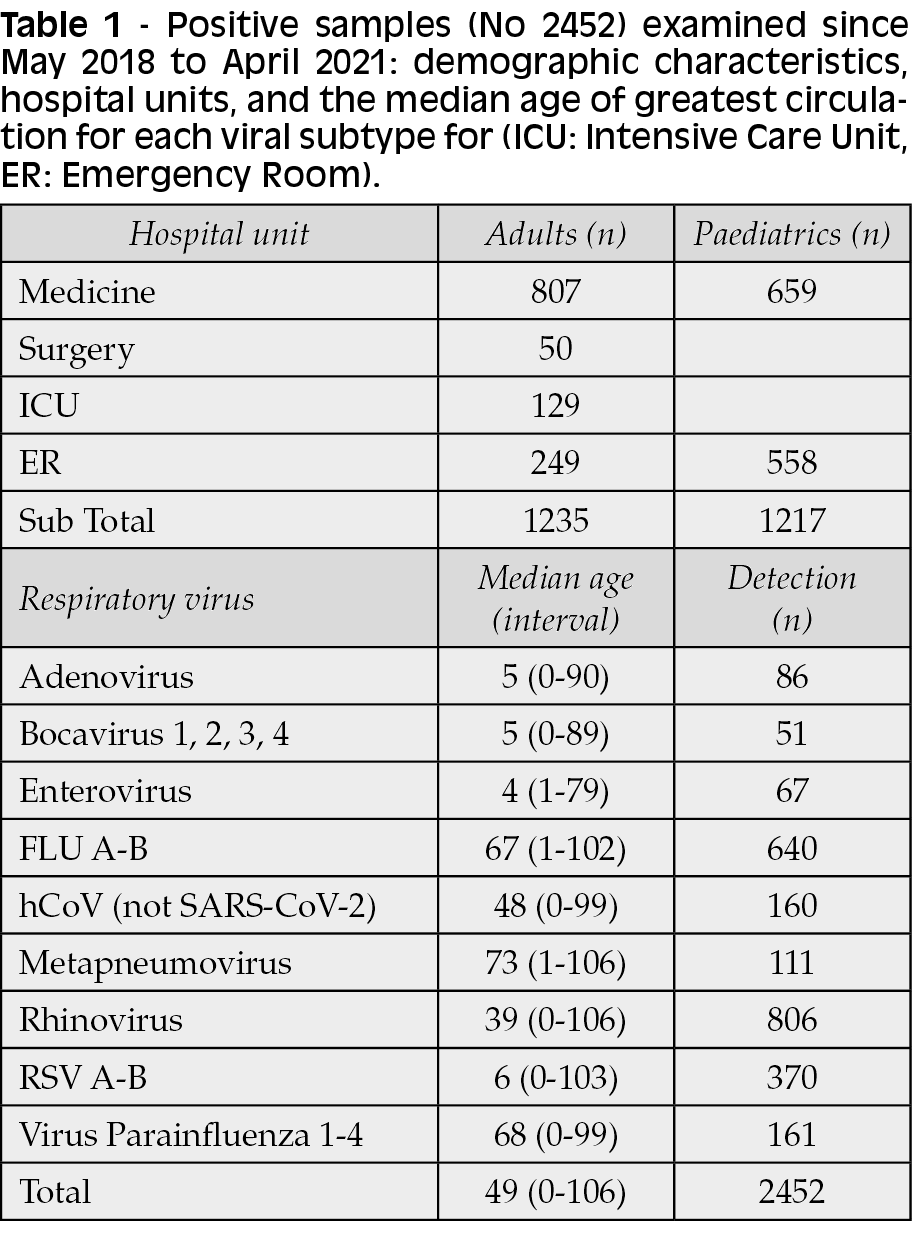
Among all 2452 positives samples, the different viruses were represented as follows: 640 Influenza virus (FLU A-B), 86 Adenovirus, 160 not-SARS-CoV-2 Coronavirus (229E, NL63, OC43), 51 Bocavirus, 67 Enterovirus, 111 Metapneumovirus, 806 Rhinovirus, 161 Parainfluenza virus, 370 respiratory syncytial virus (RSV A-B) (Table 2).

Considering that during the pandemic the number of requests for not-SARS-CoV-2 respiratory viruses dropped drastically, out of 2452 positives among all 6206 analyzed, 1094/2198 (49.8%), 1251/3211 (39%) and 107/797 (13.4%) were in 2018-2019, 2019-2020 and 2020-2021 season respectively.
As shown in Table 2 and Figure 1, the typical trend of frequency of the 2018-2019 and 2019-2020 seasons, was completely subverted in 2020-2021 (the year of the pandemic). In particular, no influenza viruses (FLU A-B) or RSVs (RSV A-B), typically winter viruses, have been detected, so we have not witnessed the typical influenza season in the winter of 2020-2021, usually dominated by FLU and RSV. Our data are confirmed by other similar reports [9, 10]. The main reasons for this lack of circulation probably lie in the strong and unexpected impact that the measures of social distancing and the use of masks in social and work environments and hand hygiene have exerted as well as, in the tight lockdown phase, the widespread implementation of mitigation measures of the community, such as the reduction of travel, the closure of schools and of some work activities.
In 2020-2021 the most common pathogen was Rhinovirus followed by Bocavirus and other Coronavirus (not SARS-CoV-2). Figure 1 shows that just a residual circulation of respiratory viruses with a less marked seasonality (Rhinoviruses) was maintained, in particular in the spring and late summer months (also in conjunction with a relaxation and restrictions, due to a low SARS-CoV-2 circulation).

Figure 1 - Total frequency (%) of virus in each flu season. The total trend of the percentage of all positive samples in the three seasons is shown at the top right.
DISCUSSION
The aim of the present study was to investigate on the possible role that restriction measures adopted to manage the COVID pandemic have had on the circulation of other respiratory viruses, comparing three consecutive flu seasons from 2018 to 2021 in our local context.
In line with other studies [9-11], our data confirm that social distancing and mask wearing profoundly influenced the spread of respiratory pathogens. Our results lead to note that the prevalence of positivity to respiratory virus infections decreased from 49.8% (2018-2019) and 39% (2019-2020) to 13.4% (2020-2021). Home isolation and implemented hygienic practices prevented the spread of viral or bacterial infection in the general population and prevented outbreaks among in-hospital population. In addition, these data would suggest the need to maintaining social distancing, mask use and hand hygiene at least in some setting such as hospital environment, or during seasonal circulation of influenza virus. We believe, at this point, it is necessary to reassess the need to maintain restrictive rules and not to focus on flu vaccination campaign only.
According to these data, the lower incidence of influenza and RSV, in light of the above, could it lead, in future, to more intense respiratory infections? Although coinfection with two or more viruses is not uncommon, competition between viruses was observed [12]. Early reports from New Zealand and Australia show an abnormal presentation of RSV in children, for example [13]. For all these reasons it may be necessary to invest in the search for highly effective vaccines against RSV and to implement vaccination strategies for the influenza virus as well. Additionally, respiratory virus surveillance can provide real-world evidence of the effectiveness of public health interventions implemented during current and future pandemics. In conclusions, viruses have always been the cause of lower respiratory tract infections and for a long time, the knowledge of the real epidemiology of respiratory viruses has been affected by the limitations of traditional culture diagnostics. In the last decade, the easier availability to use molecular and multiplex diagnostic tests has made possible to greatly change the approach to these diseases and their knowledge [8]. The COVID epidemic represents a historic moment that has enabled us to understand how crucial is to diagnose and to treat viral pneumonia adequately and promptly, and how much it can and must be done in terms of prevention to contain the circulation and spread of some viruses [6]. All these reflections leave us many challenges, which can only be addressed by continuing to closely monitor the local epidemiology of all respiratory viruses throughout the year.
Conflict of interest
The authors declare they have no conflict of interest.
Funding
None.
REFERENCES
[1] Guan WJ, Ni ZY, Hu Y, et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N Engl J Med. 2020; 382 (18), 1708-20.
[2] Giovanetti M, Benvenuto D, Angeletti S, et al. The first two cases of 2019-nCoV in Italy: Where they come from? J Med Virol. 2020; 92 (5), 518521.
[3] Cucinotta D, Vanelli M. WHO declares COVID-19 a pandemic. Acta Biomed. 2020; 91, 157-60.
[4] Vidaur L, Totorika I, Montes M, et al. Human metapneumovirus as cause of severe community-acquired pneumonia in adults: insights from a ten-year molecular and epidemiological analysis. Ann. Intensive Care. 2019; 9, 86.
[5] Leaver BA, Smith BJ, Irving L, et al. Hospitalisation, morbidity and outcomes associated with respiratory syncytial virus compared with influenza in adults of all ages Influenza Other Respir Viruses. 2021; Dec 1. Online ahead of print.
[6] Pagliano P, Sellitto C, Conti V, et al. Characteristics of viral pneumonia in the COVID-19 era: an update. Infection. 2021; 49 (4), 607-16.
[7] Groves HE, Piché-Renaud P, Peci A, et al. The impact of the COVID-19 pandemic on influenza, respiratory syncytial virus, and other seasonal respiratory virus circulation in Canada. Lancet Reg Health Am. 2021; 1, 100015.
[8] Leli C, Di Matteo L, Gotta F, et al. Prevalence of respiratory viruses by Multiplex PCR: a four-and-a-half year retrospective study in an Italian general hospital. Infez Med. 2021; 1, 94-101.
[9] Sanz-Muñoz, Tamames-Gómez S, J et al. Social Distancing, Lockdown and the Wide Use of Mask; A Magic Solution or a Double-Edged Sword for Respiratory Viruses Epidemiology? Vaccines. 2021; 9 (6), 595.
[10] Gomez GB, C, SS. Uncertain effects of the pandemic on respiratory viruses. Science. 2021; 372 (6546), 1043-4.
[11] Poole S, Brendish NJ, Clark TW, et al. SARS-CoV-2 has displaced other seasonal respiratory viruses: Results from a prospective cohort study. J Infect. 2020; 81 (6), 966-72.
[12] Trinh JT, Zeng L. Virus interactions: cooperation or competition? Future Microbiol. 2017; 12, 561-4.
[13] Foley DA, Yeoh DK, Minney-Smith CA, et al. the interseasonal resurgence of respiratory syncytial virus in Australian children following the reduction of Coronavirus Disease 2019-related public health measures. Clin Infect Dis. 2021; 73 (9), e2829-e2830.